From Surf Wiki (app.surf) — the open knowledge base
Thyroid hormones
Hormones produced by the thyroid gland
Hormones produced by the thyroid gland
File:Thyroid_system.svg|thumb|upright=1.5|The thyroid system of the thyroid hormones T3 and T4
rect 376 268 820 433 Thyroid-stimulating hormone rect 411 200 849 266 Thyrotropin-releasing hormone rect 297 168 502 200 Hypothalamus rect 66 216 386 256 Anterior pituitary gland rect 66 332 342 374 Negative feedback rect 308 436 510 475 Thyroid gland rect 256 539 563 635 Thyroid hormones rect 357 827 569 856 Catecholamine rect 399 716 591 750 Metabolism
desc bottom-left Thyroid hormones are two hormones produced and released by the thyroid gland: triiodothyronine (T3) and thyroxine (T4). They are tyrosine-based hormones that are primarily responsible for regulation of metabolism. T3 and T4 are partially composed of iodine, which is derived from food. A deficiency of iodine leads to decreased production of T3 and T4, enlarges the thyroid tissue, and causes the disease known as simple goitre.
The major form of thyroid hormone in the blood is thyroxine (T4), whose half-life of around one week is longer than that of T3. In humans, the ratio of T4 to T3 released into the blood is approximately 14:1. T4 is converted to the active T3 (three to four times more potent than T4) within cells by deiodinases (5′-deiodinase). These are further processed by decarboxylation and deiodination to produce iodothyronamine (T1a) and thyronamine (T0a). All three isoforms of the deiodinases are selenium-containing enzymes, thus dietary selenium is essential for T3 production. Calcitonin, a peptide hormone produced and secreted by the thyroid, is usually not included in the meaning of "thyroid hormone".
Thyroid hormones are one of the factors responsible for the modulation of energy expenditure. This is achieved through several mechanisms, such as mitochondrial biogenesis and adaptive thermogenesis.
American chemist Edward Calvin Kendall was responsible for the isolation of thyroxine in 1915. In 2020, levothyroxine, a manufactured form of thyroxine, was the second most commonly prescribed medication in the United States, with more than 98million prescriptions. Levothyroxine is on the World Health Organization's List of Essential Medicines.
Function
Thyroid hormones act on nearly every cell in the body. They act to increase the basal metabolic rate, affect protein synthesis, help regulate long bone growth (synergy with growth hormone) and neural maturation, and increase the body's sensitivity to catecholamines (such as norepinephrine and epinephrine) by permissiveness, especially under cold exposure. Thyroid hormones are essential to proper development and differentiation of all cells of the human body. These hormones also regulate protein, fat, and carbohydrate metabolism, affecting how human cells use energetic compounds. They also stimulate vitamin metabolism. Numerous physiological and pathological stimuli influence thyroid hormone synthesis.
Thyroid hormones lead to heat generation in humans. However, the thyronamines function via some unknown mechanism to inhibit neuronal activity; this plays an important role in the hibernation cycles of mammals and the moulting behaviour of birds. One effect of administering the thyronamines is a severe drop in body temperature.
Medical use
replacementBoth T3 and T4 are used to treat thyroid hormone deficiency (hypothyroidism). They are both absorbed well by the stomach, so they can be given orally. Levothyroxine is the chemical name of the manufactured version of T4, which is metabolised more slowly than T3 and hence usually needs only once-daily administration. Natural desiccated thyroid hormones are derived from pig thyroid glands, and are a "natural" hypothyroid treatment containing 20% T3 and traces of T2, T1 and calcitonin.
Also available are synthetic combinations of T3/T4 in different ratios (such as liotrix) and pure-T3 medications (INN: liothyronine). Levothyroxine sodium is usually the first course of treatment tried. Some patients report better outcomes with desiccated thyroid hormone; however, this is based on anecdotal evidence, and clinical trials have not shown any benefit over biosynthetic forms. Thyroid tablets are reported to have different effects, which can be attributed to the difference in torsional angles surrounding the reactive site of the molecule.
Thyronamines have no medical usages yet, though their use has been proposed for controlled induction of hypothermia, which causes the brain to enter a protective cycle and can be useful in preventing damage during ischemic shock. Synthetic thyroxine was first successfully produced by Charles Robert Harington and George Barger in 1926.
Formulations
thumb|right|Structure of (S)-thyroxine (T4) thumb|right|(S)-triiodothyronine (T3, also called [[liothyronine]])
Most people are treated with levothyroxine, or a similar synthetic thyroid hormone. Different polymorphs of the compound have different solubilities and potencies. Additionally, natural thyroid hormone supplements from the dried thyroids of animals are available. Levothyroxine contains T4 only and is therefore largely ineffective for patients unable to convert T4 to T3. These patients may choose to take natural thyroid hormone, as it contains a mixture of T4 and T3, or alternatively supplement with a synthetic T3 treatment. In these cases, synthetic liothyronine is preferred due to the potential differences between the natural thyroid products. Some studies show that mixed therapy is beneficial to all patients, but the addition of lyothyronine causes side effects, so the medication should be evaluated on an individual basis. Some natural thyroid hormone brands are FDA-approved, but others are not. Thyroid hormones are generally well tolerated. Thyroid hormones are usually not dangerous for pregnant women or nursing mothers, but should be given under a physician's supervision. In fact, if a pregnant woman with hypothyroidism is left untreated, her fetus is at a higher risk for congenital disabilities relative to the norm. When pregnant, a woman with a low-functioning thyroid will also need to increase her dosage of thyroid hormone. One exception is that thyroid hormones may aggravate heart conditions, especially in older patients; therefore, physicians may start these patients on a lower dose and work up to a larger one to avoid the risk of a heart attack.
Thyroid metabolism
synthesis
Central

-
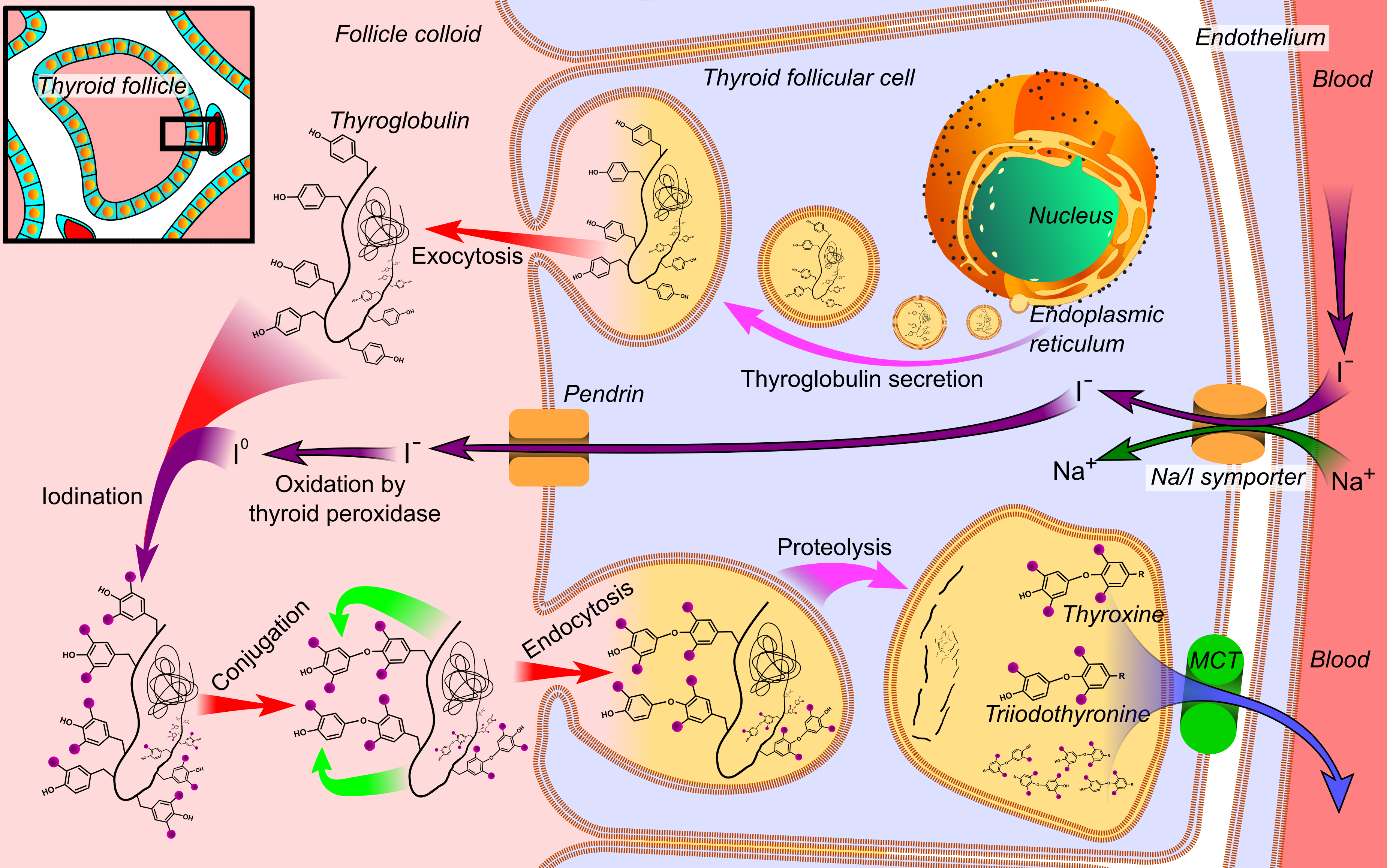
Thyroglobulin is synthesized in the rough endoplasmic reticulum and follows the secretory pathway to enter the colloid in the lumen of the thyroid follicle by exocytosis.
-
Meanwhile, a sodium-iodide (Na/I) symporter pumps iodide (I−) actively into the cell, which previously has crossed the endothelium by largely unknown mechanisms.
-
This iodide enters the follicular lumen from the cytoplasm by the transporter pendrin, in a purportedly passive manner.
-
In the colloid, iodide (I−) is oxidized to iodine (I0) by an enzyme called thyroid peroxidase.
-
Iodine (I0) is very reactive and iodinates the thyroglobulin at tyrosyl residues in its protein chain (in total containing approximately 120 tyrosyl residues).
-
In conjugation, adjacent tyrosyl residues are paired together.
-
Thyroglobulin re-enters the follicular cell by endocytosis.
-
Proteolysis by various proteases liberates thyroxine and triiodothyronine molecules
-
Efflux of thyroxine and triiodothyronine from follicular cells, which appears to be largely through monocarboxylate transporter 8 (MCT 8) and 10, and entry into the blood. ]] Thyroid hormones (T4 and T3) are produced by thyroid epithelial cells ( thyroid follicular cells) and are regulated by thyroid-stimulating hormone (TSH) made by the thyrotropes of the anterior pituitary gland. The effects of T4 in vivo are mediated via T3 (T4 is converted to T3 in target tissues). T3 is three to five times more active than T4. T4, thyroxine (3,5,3′,5′-tetraiodothyronine), is produced by follicular cells of the thyroid gland. It is produced from the precursor thyroglobulin (this is not the same as thyroxine-binding globulin [TBG]), which is cleaved by enzymes to produce active T4.
The steps in this process are as follows:
- The Na+/I− symporter transports two sodium ions across the basement membrane of the follicular cells along with an iodide ion. This is a secondary active transporter that utilises the concentration gradient of Na+ to move I− against its concentration gradient. This is called iodide trapping. Sodium is cotransported with iodide from the basolateral side of the membrane into the cell, and then concentrated in the thyroid follicles to about thirty times its concentration in the blood.
- I− is moved across the apical membrane into the colloid of the follicle by pendrin. Hydrogen peroxide is also introduced into the follicle by the action of DUX.
- Iodide is non-reactive, and the reactive I2 species is required for the next step. Thyroperoxidase (TPO) reduces hydrogen peroxide to water by transferring one electron from two I− atoms that react to form I2.
- Iodine (I2) is converted into HOI, by hydration with water. Both I2 and HOI iodinate specific tyrosyl residues of the thyroglobulin within the colloid to form 3-monoiodityrosyl (MIT-yl) and 3,5-diiodityrosyl (DIT-yl) residues—introducting iodine atoms at one or both locations ortho to the hydroxyls of tyrosine. The thyroglobulin was synthesised in the ER of the follicular cell and secreted into the colloid.
- TPO also converts tyrosyl, MIT-yl, and DIT-yl residues into their free radical forms. These forms attack other MIT-yl and DIT-yl residues. When a DIT-yl radical attacks a DIT, T4-yl (peptidic T4) is formed. When a MIT-yl radical attacks a DIT, T3-yl is formed. Other reactions are possible, but do not form physiologically active products.
- Iodinated thyroglobulin binds megalin for endocytosis back into the cell.
- TSH released from the anterior pituitary ( the adenohypophysis) binds the TSH receptor (a Gs protein-coupled receptor) on the basolateral membrane of the cell and stimulates the endocytosis of the colloid.
- The endocytosed vesicles fuse with the lysosomes of the follicular cell. The lysosomal enzymes cleave any MIT, DIT, T3, T4 as well as the inactive analogues from the iodinated thyroglobulin.
- The thyroid hormones cross the follicular cell membrane towards the blood vessels by an unknown mechanism. but recent studies indicate that monocarboxylate transporter 8 (MCT 8) and 10 play major roles in the efflux of the thyroid hormones from thyroid cells.
Thyroglobulin (Tg) is a 660 kDa, dimeric protein produced by the follicular cells of the thyroid and used entirely within the thyroid gland. Thyroxine is produced by attaching iodine atoms to the ring structures of this protein's tyrosine residues; thyroxine (T4) contains four iodine atoms, while triiodothyronine (T3), otherwise identical to T4, has one less iodine atom per molecule. The thyroglobulin protein accounts for approximately half of the protein content of the thyroid gland. Each thyroglobulin molecule contains approximately 100–120 tyrosine residues, a small number (3 and T4 are the result. Therefore, each thyroglobulin protein molecule ultimately yields very small amounts of thyroid hormone (experimentally observed to be on the order of 5–6 molecules of either T4 or T3 per original molecule of thyroglobulin).
Hydrolysis (cleavage to individual amino acids) of the modified protein by proteases then liberates T3 and T4, as well as the non-coupled tyrosine derivatives MIT and DIT. The hormones T4 and T3 are the biologically active agents central to metabolic regulation.
Peripheral
Thyroxine is believed to be a prohormone and a reservoir for the most active and main thyroid hormone, T3. T4 is converted as required in the tissues by iodothyronine deiodinase. Deficiency of deiodinase can mimic hypothyroidism due to iodine deficiency. T3 is more active than T4, though it is present in less quantity than T4.
Initiation of production in fetuses
Thyrotropin-releasing hormone (TRH) is released from hypothalamus by 6–8 gestational weeks, and thyroid-stimulating hormone (TSH) secretion from the fetal pituitary gland is evident by 12 gestational weeks; fetal production of thyroxine (T4) reaches a clinically significant level at 18–20 weeks. Fetal triiodothyronine (T3) remains low (less than 15 ng/dL) until 30 weeks of gestation, and increases to 50 ng/dL at term.
Iodine deficiency
Among humans with dietary iodine deficiency, the thyroid will not be able to make thyroid hormones. The lack of thyroid hormones will lead to decreased negative feedback on the pituitary gland, leading to increased production of thyroid-stimulating hormone, which causes the thyroid to enlarge in a medical condition called endemic colloid goitre. This has the effect of increasing the thyroid's ability to trap more iodide, compensating for the iodine deficiency and allowing it to produce adequate amounts of thyroid hormone.
Circulation and transport
Plasma transport
Most of the thyroid hormone circulating in the blood is bound to transport proteins, and only a very small fraction is unbound and biologically active. Therefore, measuring concentrations of free thyroid hormones is important for diagnosis, while measuring total levels can be misleading.
Thyroid hormone in the blood is usually distributed as follows:
| Type | Percent | |
|---|---|---|
| bound to thyroxine-binding globulin (TBG) | ||
| bound to transthyretin or "thyroxine-binding prealbumin" (TTR or TBPA) | ||
| albumin | ||
| unbound T4 (fT4) | ||
| unbound T3 (fT3) |
Despite being lipophilic, T3 and T4 cross the cell membrane via carrier-mediated transport, which is ATP-dependent.
T1a and T0a are positively charged and do not cross the membrane; they are believed to function via the trace amine-associated receptor (TAR1, TA1), a G-protein-coupled receptor located in the cytoplasm.
Another critical diagnostic tool is measurement of the amount of thyroid-stimulating hormone (TSH) that is present.
Membrane transport
Contrary to common belief, thyroid hormones cannot traverse cell membranes in a passive manner like other lipophilic substances. The iodine in o-position makes the phenolic OH-group more acidic, resulting in a negative charge at physiological pH. However, at least 10 different active, energy-dependent and genetically regulated iodothyronine transporters have been identified in humans. They guarantee that intracellular levels of thyroid hormones are higher than in blood plasma or interstitial fluids.
Intracellular transport
Little is known about intracellular kinetics of thyroid hormones. However, recently it could be demonstrated that the crystallin CRYM binds 3,5,3′-triiodothyronine in vivo.
Mechanism of action
Main article: Thyroid hormone receptor
The thyroid hormones function via a well-studied set of nuclear receptors, termed the thyroid hormone receptors. These receptors, together with corepressor molecules, bind DNA regions called thyroid hormone response elements (TREs) near genes. This receptor-corepressor-DNA complex can block gene transcription. Triiodothyronine (T3), which is the active form of thyroxine (T4), goes on to bind to receptors. The deiodinase catalyzed reaction removes an iodine atom from the 5′ position of the outer aromatic ring of thyroxine's (T4) structure. When triiodothyronine (T3) binds a receptor, it induces a conformational change in the receptor, displacing the corepressor from the complex. This leads to recruitment of coactivator proteins and RNA polymerase, activating transcription of the gene. Although this general functional model has considerable experimental support, there remain many open questions.
More recently genetic evidence has been obtained for a second mechanism of thyroid hormone action involving one of the same nuclear receptors, TRβ, acting rapidly in the cytoplasm through the PI3K. This mechanism is conserved in all mammals but not fish or amphibians, and regulates brain development and adult metabolism. The mechanism itself parallels the actions of the nuclear receptor in the nucleus: in the absence of hormone, TRβ binds to PI3K and inhibits its activity, but when hormone binds the complex dissociates, PI3K activity increases, and the hormone bound receptor diffuses into the nucleus.
Thyroxine, iodine and apoptosis
Thyroxine and iodine stimulate the apoptosis of the cells of the larval gills, tail and fins in amphibian metamorphosis, and stimulate the evolution of their nervous system transforming the aquatic, vegetarian tadpole into the terrestrial, carnivorous frog. In fact, amphibian frog Xenopus laevis serves as an ideal model system for the study of the mechanisms of apoptosis.
Effects of triiodothyronine
Effects of triiodothyronine (T3) which is the metabolically active form:
- Increases cardiac output
- Increases heart rate
- Increases ventilation rate
- Increases basal metabolic rate
- Potentiates the effects of catecholamines (i.e. increases sympathetic activity)
- Potentiates brain development
- Thickens endometrium in females
- Increases catabolism of proteins and carbohydrates
Measurement
Further information: Thyroid function tests
Triiodothyronine (T3) and thyroxine (T4) can be measured as free T3 and free T4, which are indicators of their activities in the body. They can also be measured as total T3 and total T4, which depend on the amount that is bound to thyroxine-binding globulin (TBG). A related parameter is the free thyroxine index, which is total T4 multiplied by thyroid hormone uptake, which, in turn, is a measure of the unbound TBG. Additionally, thyroid disorders can be detected prenatally using advanced imaging techniques and testing fetal hormone levels.
Anti-thyroid drugs
Iodine uptake against a concentration gradient is mediated by a sodium–iodine symporter and is linked to a sodium-potassium ATPase. Perchlorate and thiocyanate are drugs that can compete with iodine at this point. Compounds such as goitrin, carbimazole, methimazole, propylthiouracil can reduce thyroid hormone production by interfering with iodine oxidation.
References
References
- References used in image are found in image article in Commons:[[Commons:File:Thyroid system.png#References]].
- (21 October 2019). "How Your Thyroid Works". endocrineweb.com.
- Ijaz Ahsan. (1997). "Textbook of Surgery". CRC Press.
- "How long does thyroxine stay in your system?".
- (23 April 2014). "Thyroid Hormone Toxicity". WedMD LLC.
- (April 1990). "Thyroidal and peripheral production of 3,5,3'-triiodothyronine in humans by multicompartmental analysis". The American Journal of Physiology.
- (April 2022). "Hypothalamic control of energy expenditure and thermogenesis". Experimental & Molecular Medicine.
- "1926 Edward C Kendall". American Society for Biochemistry and Molecular Biology.
- "The Top 300 of 2020".
- "Levothyroxine - Drug Usage Statistics".
- (2019). "World Health Organization model list of essential medicines: 21st list 2019". World Health Organization.
- (2022). "StatPearls". StatPearls Publishing.
- (July 2006). "Thyroxine-triiodothyronine combination therapy versus thyroxine monotherapy for clinical hypothyroidism: meta-analysis of randomized controlled trials". The Journal of Clinical Endocrinology and Metabolism.
- (October 2015). "Thyroid hormones--From Crystal Packing to Activity to Reactivity". Angewandte Chemie.
- Robert Lloyd Segal, MD Endocrinologist
- "preferred thyroid hormone --Levothyroxine Sodium (Synthroid, Levoxyl, Levothroid, Unithroid)". MedicineNet.com.
- "Hypothyroidism Causes, Symptoms, Diagnosis, Treatment Information Produced by Medical Doctors". MedicineNet.com.
- (September 2015). "Structure Elucidation and Characterization of Different Thyroxine Polymorphs". Angewandte Chemie.
- (May 1989). "Thyroid hormone treatment: new insights into an old therapy". JAMA.
- (2004). "Synthetic Thyroxine vs Desiccated Thyroid -Reply (citing Cooper, DS, above)". JAMA: The Journal of the American Medical Association.
- (2001). "Thyroid hormone replacement therapy". Hormone Research.
- [http://thyroid.about.com/od/thyroiddrugstreatments/a/refusingmeds.htm "Consequences of Not Taking Thyroid Medications - Implications of Failing to Take Prescription Thyroid Drugs"] {{Webarchive. link. (16 February 2009 , Retrieved on 27 March 2009)
- [http://www.armourthyroid.com/ "Armour Thyroid"], Retrieved on 1 April 2009
- [http://www.nature-throid.com/ "Nature-Throid"], Retrieved on 1 April 2009
- [http://thyroid.about.com/b/2008/09/10/armour-thyroid-shortages-worsening-what-can-thyroid-patients-do.htm "Armour Thyroid Shortages Worsening: What Can Thyroid Patients Do?"] {{Webarchive. link. (3 March 2009 , Retrieved on 27 March 2009)
- [https://web.archive.org/web/20100628160635/http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0000685 Liothyronine]
- (January 2015). "Treatment of hypothyroidism with levothyroxine or a combination of levothyroxine plus L-triiodothyronine". Best Practice & Research. Clinical Endocrinology & Metabolism.
- [http://www.usdoctor.com/thyroid.htm "Thyroid Information"] {{Webarchive. link. (27 February 2012 , Retrieved on 27 March 2009)
- (March 1994). "Desiccated thyroid in a nutritional supplement". The Journal of Family Practice.
- [http://drugs.emedtv.com/nature-throid/nature-throid.html "Nature-Throid"] {{Webarchive. link. (15 February 2009 , Retrieved on 1 April 2009)
- (April 2016). "Medical Physiology". Elsevier/Saunders.
- (28 March 2024). "Endocrinology: An Integrated Approach". BIOS Scientific Publishers.
- (January 2010). "Iodine, Iodine metabolism and Iodine deficiency disorders revisited". Indian Journal of Endocrinology and Metabolism.
- (2001). "Iodide handling by the thyroid epithelial cell". Experimental and Clinical Endocrinology & Diabetes.
- (August 2021). "The PDZ protein SCRIB regulates sodium/iodide symporter (NIS) expression at the basolateral plasma membrane". FASEB Journal.
- (Jul 2008). "Factors influencing the study of peroxidase-generated iodine species and implications for thyroglobulin synthesis". Thyroid.
- (January 2010). "Iodine, Iodine metabolism and Iodine deficiency disorders revisited". Indian Journal of Endocrinology and Metabolism.
- (2000). "Endotext". MDText.com, Inc..
- (November 2015). "Coupling of chromophores with exactly opposite luminescence behaviours in mesostructured organosilicas for high-efficiency multicolour emission". Chemical Science.
- (May 1995). "Importance of the content and localization of tyrosine residues for thyroxine formation within the N-terminal part of human thyroglobulin". European Journal of Endocrinology.
- (2005). "The effect of hydrolysis time on amino acid analysis". Journal of AOAC International.
- (2003). "Effects of hydrolysis on the delta13C values of individual amino acids derived from polypeptides and proteins". Rapid Communications in Mass Spectrometry.
- (2 May 2003). "Human Anatomy & Physiology, Sixth Edition". Benjamin Cummings.
- (June 2008). "Effective cellular uptake and efflux of thyroid hormone by human monocarboxylate transporter 10". Molecular Endocrinology.
- (August 2011). "Molecules important for thyroid hormone synthesis and action - known facts and future perspectives". Thyroid Research.
- (2019). "Diagnostic Immunohistochemistry". Elsevier.
- (June 1977). "Triiodothyronine, thyroxine, and iodine in purified thyroglobulin from patients with Graves' disease". The Journal of Clinical Investigation.
- (July 2022). "Maintaining the thyroid gland in mutant thyroglobulin-induced hypothyroidism requires thyroid cell proliferation that must continue in adulthood". The Journal of Biological Chemistry.
- Boron, W.F.. (2003). "Medical Physiology: A Cellular And Molecular Approach". Elsevier/Saunders.
- (March 2020). "Tyrosinase-Mediated Oxidative Coupling of Tyrosine Tags on Peptides and Proteins". Journal of the American Chemical Society.
- (September 2012). "Mechanisms of thyroid hormone action". The Journal of Clinical Investigation.
- (June 2010). "The Challenges and Complexities of Thyroid Hormone Replacement". Laboratory Medicine.
- (March 2009). "Minireview: Defining the roles of the iodothyronine deiodinases: current concepts and challenges". Endocrinology.
- (2011). "Oxford Textbook of Endocrinology and Diabetes". Oxford University Press.
- (2011). "Oxford Textbook of Endocrinology and diabetes". Oxford University Press.
- (2004). "Pediatric endocrinology: mechanisms, manifestations and management". Lippincott Williams & Wilkins.
- (April 2003). "Transplacental thyroxine and fetal brain development". The Journal of Clinical Investigation.
- (April 2015). "Iodine deficiency and thyroid disorders". The Lancet. Diabetes & Endocrinology.
- (5 April 2017). "Henry's clinical diagnosis and management by laboratory methods". Elsevier Health Sciences.
- (June 1987). "Physiological aspects of the thyroid trapping function and its suppression in iodine deficiency using 99mTc pertechnetate". Acta Endocrinologica.
- (August 2001). "Plasma membrane transport of thyroid hormones and its role in thyroid hormone metabolism and bioavailability". Endocrine Reviews.
- (August 2008). "[Absorption, transport and bio-availability of iodothyronines]". Deutsche Medizinische Wochenschrift.
- (April 2007). "micro-Crystallin as an intracellular 3,5,3'-triiodothyronine holder in vivo". Molecular Endocrinology.
- (April 2014). "Thyroid hormone regulation of metabolism". Physiological Reviews.
- (August 2000). "Gene regulation by thyroid hormone". Trends in Endocrinology and Metabolism.
- (2014). "Genome-wide binding patterns of thyroid hormone receptor beta". PLOS ONE.
- (September 2014). "A rapid cytoplasmic mechanism for PI3 kinase regulation by the nuclear thyroid hormone receptor, TRβ, and genetic evidence for its role in the maturation of mouse hippocampal synapses in vivo". Endocrinology.
- (December 2017). "Noncanonical thyroid hormone signaling mediates cardiometabolic effects in vivo". Proceedings of the National Academy of Sciences of the United States of America.
- (2014). "Optogenetic Control of Apoptosis in Targeted Tissues of Xenopus laevis Embryos". Journal of Cell Death.
- Venturi, Sebastiano. (2011). "Evolutionary Significance of Iodine". Current Chemical Biology.
- (2014). "Iodine, PUFAs and Iodolipids in Health and Disease: An Evolutionary Perspective". Human Evolution.
- (June 2015). "Apoptosis and differentiation of Xenopus tail-derived myoblasts by thyroid hormone". Journal of Molecular Endocrinology.
- (June 1987). "Catabolic effects of thyroid hormone excess: the contribution of adrenergic activity to hypermetabolism and protein breakdown". Metabolism.
- (January 2002). "Case finding and screening strategies for thyroid dysfunction". Clinica Chimica Acta; International Journal of Clinical Chemistry.
- [http://www.brooksidepress.org/Products/Military_OBGYN/Lab/ThyroidFunctionTests.htm Military Obstetrics & Gynecology > Thyroid Function Tests] In turn citing: Operational Medicine 2001, Health Care in Military Settings, NAVMED P-5139, 1 May 2001, Bureau of Medicine and Surgery, Department of the Navy, 2300 E Street NW, Washington, D.C., 20372-5300
- (March 2014). "Fetal thyroïdology". Best Practice & Research. Clinical Endocrinology & Metabolism.
- (January 1998). "The role of thyroid hormones in depression". European Journal of Endocrinology.
- (December 1996). "Thyroid hormones as neurotransmitters". Thyroid.
- (June 2019). "Thyroid and Cardiovascular Disease: Research Agenda for Enhancing Knowledge, Prevention, and Treatment". Circulation.
- Parry CH. Elements of Pathology and Therapeutics, Being the Outlines of a Work. Bath, England: R. Cruttwell, 1815.
- "Myopathies associated with thyroid disease".
- (September 2020). "Endocrine myopathies: clinical and histopathological features of the major forms". Acta Myologica.
- (April 1986). "Effect of hyperthyroidism on fibre-type composition, fibre area, glycogen content and enzyme activity in human skeletal muscle". Clinical Physiology.
- (July 2014). "Myopathies of endocrine disorders: A prospective clinical and biochemical study". Annals of Indian Academy of Neurology.
- (2023). "StatPearls". StatPearls Publishing.
- (January 1989). "Effects of hypothyroidism on the sensitivity of glycolysis and glycogen synthesis to insulin in the soleus muscle of the rat". The Biochemical Journal.
- (2019-01-01). "Neuroradiology". Elsevier.
- (June 2010). "Role of late maternal thyroid hormones in cerebral cortex development: an experimental model for human prematurity". Cerebral Cortex.
- (January 2016). "Association of maternal thyroid function during early pregnancy with offspring IQ and brain morphology in childhood: a population-based prospective cohort study". The Lancet. Diabetes & Endocrinology.
- (March 2014). "Genetics of normal and abnormal thyroid development in humans". Best Practice & Research. Clinical Endocrinology & Metabolism.
- (September 1993). "Normal circulating triiodothyronine concentrations are maintained despite severe hypothyroidism in growing pigs fed rapeseed presscake meal". The Journal of Nutrition.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Thyroid hormones — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report