From Surf Wiki (app.surf) — the open knowledge base
Signs and symptoms of multiple sclerosis
Neurological signs and symptoms
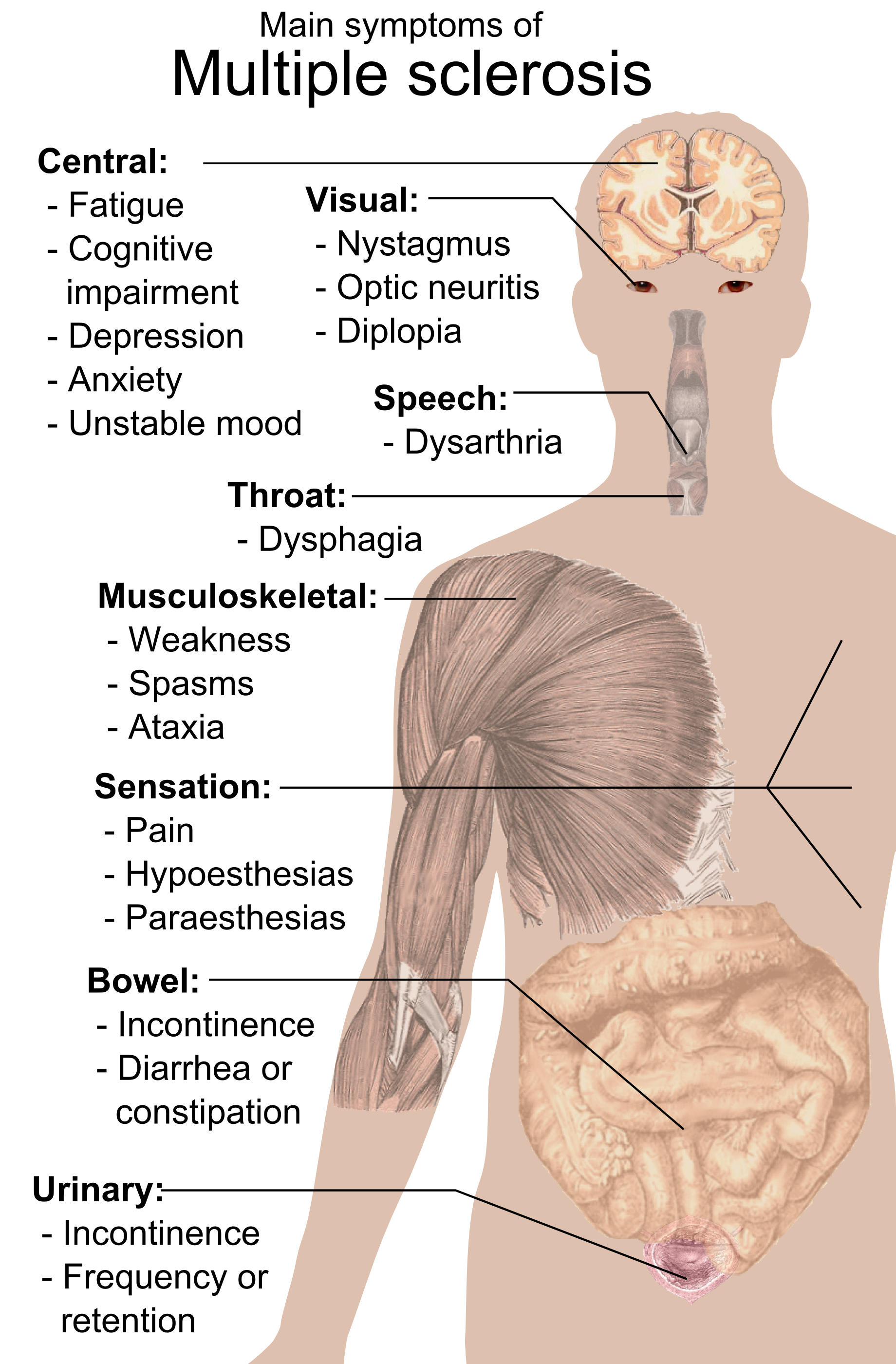
Neurological signs and symptoms


Multiple sclerosis can cause a variety of symptoms varying significantly in severity and progression among individuals: changes in sensation (hypoesthesia), muscle weakness, abnormal muscle spasms, or difficulty moving; difficulties with coordination and balance; problems in speech (dysarthria) or swallowing (dysphagia), visual problems (nystagmus, optic neuritis, phosphenes or diplopia), fatigue and acute or chronic pain syndromes, bladder and bowel difficulties, cognitive impairment, or emotional symptomatology (mainly major depression). The main clinical measure in progression of the disability and severity of the symptoms is the Expanded Disability Status Scale or EDSS.
The initial attacks are often transient, mild (or asymptomatic), and self-limited. They often do not prompt a health care visit and sometimes are only identified in retrospect once the diagnosis has been made after further attacks. The most common initial symptoms reported are: changes in sensation in the arms, legs or face (33%), complete or partial vision loss (optic neuritis) (20%), weakness (13%), double vision (7%), unsteadiness when walking (5%), and balance problems (3%); but many rare initial symptoms have been reported such as aphasia or psychosis. Fifteen percent of individuals have multiple symptoms when they first seek medical attention.
Fatigue
Fatigue is very common and disabling in MS. Some 65% of people with MS experience fatigue symptomatology, and of these some 15-40% report fatigue as their most disabling MS symptom. A 2023 study found that effect on fatigue was the most valued attribute of MS therapy, and that participants would accept six additional relapses in 2 years and a decrease of 7 years in time to disease progression to improve either cognitive or physical fatigue from "quite a bit of difficulty" to "no difficulty."
The pathophysiology and mechanisms causing MS fatigue are not well understood.
MS fatigue can be affected by body heat and this may differentiate MS fatigue from other primary fatigue.
Perceived fatigue and fatigability (loss of strength) are regarded independently. Primary MS fatigue is sometimes called "lassitude". MS fatigue may reduce during periods of other MS symptom remission.
Knowledge of MS fatigue pathophysiology, diagnosis and treatment is very limited.
Primary vs. secondary
In some areas it has been proposed that fatigue be separated into primary fatigue, caused directly by a disease process, and secondary fatigue, caused by more general impacts on the person of having a disease (such as disrupted sleep).
Contributory factors to secondary fatigue
Factors such as disturbed sleep, chronic pain, poor nutrition, or even some medications can all contribute to secondary fatigue and medical professionals are encouraged to identify and modify them.
Association with depression
Early 2000s commentary saw a close relationship of secondary fatigue with depressive symptomatology. When depression is reduced fatigue also tends to reduce and it is recommended that patients should be evaluated for depression before other therapeutic approaches are used.
Correlation with brain changes
Studies have found MS fatigue correlates, not with lesion volume or brain atrophy, but with damage to NAWM (normal appearing white matter) (which will not show on normal MRI but will show on DTI (diffusion tensor imaging)). The correlation becomes unreliable due to ageing in patients aged over 65.
A 2008 study found MS fatigue correlated with lesion load and brain atrophy.
A 2024 study found results suggested that fatigue was not driven by neuroinflammation or neurodegeneration measurable by current structural MRI in early RRMS.
Medications
Medications used to treat MS fatigue include amantadine, pemoline, methylphenidate, and modafinil, as well as cognitive behavioral therapy (CBT) and psychological interventions of energy conservation; but their effects are limited. For these reasons fatigue is a difficult symptom to manage.
Technology
As of 2022 apps were being experimented with in the field of MS fatigue.
Bladder and bowel
Bladder problems appear in 70–80% of people with multiple sclerosis (MS) and they have an important effect both on hygiene habits and social activity. Bladder problems are usually related with high levels of disability and pyramidal signs in lower limbs.
The most common problems are an increase in frequency and urgency (incontinence) but difficulties to begin urination, hesitation, leaking, sensation of incomplete urination, and retention also appear. When retention occurs secondary urinary infections are common.
There are many cortical and subcortical structures implicated in urination and MS lesions in various central nervous system structures can cause these kinds of symptoms.
Treatment objectives are the alleviation of symptoms of urinary dysfunction, treatment of urinary infections, reduction of complicating factors and the preservation of renal function. Treatments can be classified in two main subtypes: pharmacological and non-pharmacological. Pharmacological treatments vary greatly depending on the origin or type of dysfunction and some examples of the medications used are: alfuzosin for retention, trospium and flavoxate for urgency and incontinency, and desmopressin for nocturia.{{cite web | work = MedlinePlus | publisher = U.S. National Library of Medicine | title = Desmopressin Non pharmacological treatments involve the use of pelvic floor muscle training, stimulation, biofeedback, pessaries, bladder retraining, and sometimes intermittent catheterization.
Bowel problems affect around 70% of patients. Around 50% of patients experience constipation and up to 30% experience fecal incontinence. Cause of bowel impairments in MS patients is usually either a reduced gut motility or an impairment in neurological control of defecation. The former is commonly related to immobility or secondary effects from drugs used in the treatment of the disease. Pain or problems with defecation can be helped with a diet change which includes among other changes an increased fluid intake, oral laxatives or suppositories and enemas when habit changes and oral measures are not enough to control the problems.
Cognitive deficits
Deficits
Some of the most common deficits affect recent memory, attention, processing speed, visual-spatial abilities and executive function. Symptoms related to cognition include emotional instability and fatigue including neurological fatigue. Cognitive deficits are independent of physical disability and can occur in the absence of neurological dysfunction.
Appraisal
Reviews have recommended annual appraisal using the Symbol Digit Modalities Test (SDMT) or similarly validated test.
Effects
Severe cognitive impairment is a major predictor of a low quality of life, unemployment, caregiver distress, and difficulty in driving; limitations in a patient's social and work activities are also correlated with the extent of impairment.
Prevalence
Cognitive impairments occur in about 40 to 60 percent of patients with multiple sclerosis, with the lowest percentages usually from community-based studies and the highest ones from hospital-based.
Impairments may be present at the beginning of the disease. Probable multiple sclerosis patients, meaning after a first attack but before a secondary confirmatory one, have up to 50 percent of patients with impairment at onset. Dementia is rare and occurs in only five percent of patients.
Causation
Cognitive deficits have been linked to greater lesion load, white matter lesion location, microstructural injury, gray matter lesions, cortical and subcortical gray matter brain atrophy, and discrepant patterns of cerebral activation. Measures of tissue atrophy are well correlated with, and predict, cognitive dysfunction. Neuropsychological outcomes are highly correlated with linear measures of sub-cortical atrophy. Cognitive impairment is the result of not only tissue damage, but tissue repair and adaptive functional reorganization.
Postulated treatments
As of 2018 efficacy of possible interventions was low, inconclusive, or preliminary. Neuropsychological rehabilitation may help to reverse or decrease the cognitive deficits although studies on the issue have been of low quality. Acetylcholinesterase inhibitors are commonly used to treat Alzheimer's disease related dementia and so are thought to have potential in treating the cognitive deficits in multiple sclerosis. They have been found to be effective in preliminary clinical trials.
Prevention
Primary prevention by interventions and healthy lifestyles that promote brain maintenance has been proposed.
Emotional
Emotional symptoms are also common and are thought to be both a normal response to having a debilitating disease and the result of damage to specific areas of the central nervous system that generate and control emotions.
Clinical depression is the most common neuropsychiatric condition: lifetime depression prevalence rates of 40–50% and 12-month prevalence rates around 20% have been typically reported for samples of people with MS; these figures are considerably higher than those for the general population or for people with other chronic illnesses. Brain imaging studies trying to relate depression to lesions in certain regions of the brain have met with variable success. On balance the evidence seems to favour an association with neuropathology in the left anterior temporal/parietal regions.
Other feelings such as anger, anxiety, frustration, and hopelessness also appear frequently. Suicide is a possibility, since it accounts for 15% of MS deaths.
Rarely psychosis may also be featured.
Internuclear ophthalmoplegia
Main article: Internuclear ophthalmoplegia
Internuclear ophthalmoplegia is a disorder of conjugate lateral gaze. The affected eye shows impairment of adduction. The partner eye diverges from the affected eye during abduction, producing diplopia; during extreme abduction, compensatory nystagmus can be seen in the partner eye. Diplopia means double vision while nystagmus is involuntary eye movement characterized by alternating smooth pursuit in one direction and a saccadic movement in the other direction.
Internuclear ophthalmoplegia occurs when MS affects a part of the brain stem called the medial longitudinal fasciculus, which is responsible for communication between the two eyes by connecting the abducens nucleus of one side to the oculomotor nucleus of the opposite side. This results in the failure of the medial rectus muscle to contract appropriately, so that the eyes do not move equally (called disconjugate gaze).
Different drugs as well as optic compensatory systems and prisms can be used to improve these symptoms. Surgery can also be used in some cases for this problem.
Mobility restrictions
_Animation_all_rows.gif)
Restrictions in mobility (walking, transfers, bed mobility etc.) are common in individuals with multiple sclerosis. Although this is not something constant it can happen when experiencing a flare up. Within 10 years after the onset of MS one-third of patients reach a score of 6 on the Expanded Disability Status Scale (EDSS), requiring the use of a unilateral walking aid, and by 30 years the proportion increases to 83%. Within five years of onset the EDSS is six in 50% of those with the progressive form of MS.
A wide range of impairments may exist in people with MS, which can act either alone or in combination to impact directly on a person's balance, function and mobility. Such impairments include fatigue, weakness, hypertonicity, low exercise tolerance, impaired balance, ataxia and tremor.
Interventions may be aimed at the individual impairments that reduce mobility or at the level of disability. This second level intervention includes provision, education, and instruction in the use of equipment such as walking aids, wheelchairs, motorized scooters and car adaptations as well as instruction on compensatory strategies to accomplish an activity — for example undertaking safe transfers by pivoting in a flexed posture rather than standing up and stepping around.
Optic neuritis
Main article: Optic neuritis
Up to 50% of patients with MS will develop an episode of optic neuritis and 20% of the time optic neuritis is the presenting sign of MS. The presence of demyelinating white matter lesions on brain MRIs at the time of presentation for optic neuritis is the strongest predictor in developing clinical diagnosis of MS. Almost half of patients with optic neuritis have white matter lesions consistent with multiple sclerosis.
At five year follow-ups the overall risk of developing MS is 30%, with or without MRI lesions. Patients with a normal MRI still develop MS (16%), but at a lower rate compared to those patients with three or more MRI lesions (51%). From the other perspective, however, 44% of patients with any demyelinating lesions on MRI at presentation will not have developed MS ten years later.
Individuals experience rapid onset of pain in one eye followed by blurry vision in part or all its visual field. Flashes of light (phosphenes) may also be present. Inflammation of the optic nerve causes loss of vision most usually by the swelling and destruction of the myelin sheath covering the optic nerve.
The blurred vision usually resolves within 10 weeks but individuals are often left with less vivid color vision, especially red, in the affected eye.
A systemic intravenous treatment with corticosteroids may quicken the healing of the optic nerve, prevent complete loss of vision and delay the onset of other symptoms.
Asymmetry in thickness of RNFL as indicator of optic neuritis in MS
Asymmetry between the eyes in thickness of RNFL has been proposed as a strong indicator of optic neuritis in MS. RNFL data may indicate the pace of future development of the MS.
Pain
Pain is a common symptom in MS. A 2013 study which systematically pooled results from 28 studies (7101 patients) estimated that pain affected 63% of people with MS. These 28 studies described pain in a large range of different people with MS. The authors found no evidence that pain was more common in people with progressive types of MS, in females compared to males, in people with different levels of disability, or in people who had had MS for different periods of time.
MS pain can be
- neuropathic (nerve) pain directly caused by MS. A lesion in the brain or spinal cord can cause nerves to fire inappropriately. Neuropathic pain is most commonly steady, and described as burning, tight, tingling, nagging, aching, throbbing, or even icy. However neuropathic pain can also be intermittent, and described as shooting, stabbing, or lightning bolt-like. Other unpleasant sensations may also occur.
- musculoskeletal (muscle/bone) pain, caused when muscles, bones, or joints experience decreased mobility, prolonged sitting, spasms, and other improper use and disuse.
MS patients may also be experiencing pain from comorbidity causes.
Pain can be severe and debilitating, and can have a profound effect on the quality of life and mental health of those affected. Certain types of pain are thought to sometimes appear after a lesion to the ascending or descending tracts that control the transmission of painful stimulus, such as the anterolateral system, but many other causes are also possible. The most prevalent types of pain are thought to be headaches (43%), dysesthetic limb pain (26%), back pain (20%), painful spasms (15%) such as the MS Hug, painful Lhermitte's phenomenon (16%) and Trigeminal Neuralgia (3%). These authors did not however find enough data to quantify the prevalence of painful optic neuritis.
Acute pain is mainly due to optic neuritis, trigeminal neuralgia, Lhermitte's sign or dysesthesias. Subacute pain is usually secondary to the disease and can be a consequence of spending too much time in the same position, urinary retention, or infected skin ulcers. Chronic pain is common and harder to treat.
Trigeminal neuralgia
Trigeminal neuralgia (or "tic douloureux") is a disorder of the trigeminal nerve that causes episodes of intense pain in the eyes, lips, nose, scalp, forehead, and jaw, affecting 2-4% of MS patients. The episodes of pain occur paroxysmally (suddenly) and the patients describe it as trigger area on the face, so sensitive that touching or even air currents can bring an episode of pain. Usually it is successfully treated with anticonvulsants such as carbamazepine, or phenytoin although others such as gabapentin can be used. When drugs are not effective, surgery may be recommended. Glycerol rhizotomy (surgical injection of glycerol into a nerve) has been studied although the beneficial effects and risks in MS patients of the procedures that relieve pressure on the nerve are still under discussion.
Lhermitte's sign
Lhermitte's sign is an electrical sensation that runs down the back and into the limbs and is produced by bending the neck forward. The sign suggests a lesion of the dorsal columns of the cervical cord or of the caudal medulla, correlating significantly with cervical MRI abnormalities. Between 25 and 40% of MS patients report having Lhermitte's sign during the course of their illness. It is not always experienced as painful, but about 16% of people with MS will experience painful Lhermitte's sign.
Dysesthesias
Dysesthesias are disagreeable sensations produced by ordinary stimuli. The abnormal sensations are caused by lesions of the peripheral or central sensory pathways, and are described as painful feelings such as burning, wetness, itching, electric shock or pins and needles. Both Lhermitte's sign and painful dysesthesias usually respond well to treatment with carbamazepine, clonazepam or amitriptyline. A related symptom is a pleasant, yet unsettling sensation which has no normal explanation (such as sensation of gentle warmth arising from touch by clothing).
Reduced sense of smell
People with multiple sclerosis have been found to have reduced sense of smell, including lower olfactory thresholds.
Sexual
Sexual dysfunction is one of many symptoms affecting persons with a diagnosis of MS. Sexual dysfunction in men encompasses both erectile and ejaculatory disorder. The prevalence of sexual dysfunction in men with MS ranges from 75 to 91%. Erectile dysfunction appears to be the most common issue documented in MS. It is thought to be due to alteration of the ejaculatory reflex which can be affected by neurological conditions such as MS. Sexual dysfunction is also prevalent in female MS patients, typically lack of orgasm, probably related to disordered genital sensation.
Spasticity and spasms
.jpg)
Spasticity is characterised by involuntary muscle movements (spasms), muscle stiffness, pain and restriction with certain movements or positions (causing difficulty in performing some activities), and a change in mobility or upper limb function.
Spasms affect about 15% of people with MS overall.
A physiotherapist can help to reduce spasticity and avoid the development of contractures with techniques such as passive stretching. There is evidence, albeit limited, of the clinical effectiveness of THC and CBD extracts, baclofen, dantrolene, diazepam, and tizanidine. In the most complicated cases intrathecal injections of baclofen can be used. There are also palliative measures like castings, splints or customized seatings.
Speech and swallowing
Speech problems include slurred speech, decreased talking speed, and problems with articulation of sounds (dysarthria). Low tone of voice (dysphonia) may be caused by changes in diaphragm control.
A related problem, since it involves similar anatomical structures, is swallowing difficulties (dysphagia).
Transverse myelitis
Main article: Transverse myelitis
Some MS patients develop rapid onset of numbness, weakness, bowel or bladder dysfunction, and/or loss of muscle function, typically in the lower half of the body. This is the result of MS attacking the spinal cord. The symptoms and signs depend upon the nerve cords involved and the extent of the involvement.
Prognosis for complete recovery is generally poor. Recovery from transverse myelitis usually begins between weeks 2 and 12 following onset and may continue for up to 2 years in some patients and as many as 80% of individuals with transverse myelitis are left with lasting disabilities.
Though it was considered for many years that traverse myelitis was a normal consequence of MS, since the discovery of anti-AQP4 and anti-MOG biomarkers it is not. Now TM is considered an indicator of neuromyelitis optica, and a red flag against the diagnosis of MS.
Tremor and ataxia
Main article: Tremor
Tremor is an unintentional, somewhat rhythmic, muscle movement involving to-and-fro movements (oscillations) of one or more parts of the body. It is the most common of all involuntary movements and can affect the hands, arms, head, face, vocal cords, trunk, and legs. Ataxia is an unsteady and clumsy motion of the limbs or torso due to a failure of the gross coordination of muscle movements. People with ataxia experience a failure of muscle control in their arms and legs, resulting in a lack of balance and coordination or a disturbance of gait.
Tremor and ataxia are frequent in MS and present in 25 to 60% of patients. They can be very disabling and embarrassing, and are difficult to manage. The origin of tremor in MS is difficult to identify but it can be due to a mixture of different factors such as damage to the cerebellar connections, weakness, spasticity, etc.
Many medications have been proposed to treat tremor; however their efficacy is very limited. Medications that have been reported to provide some relief are isoniazid, carbamazepine, propranolol and gluthetimide but published evidence of effectiveness is limited. Physical therapy is not indicated as a treatment for tremor or ataxia although the use of orthese devices can help. An example is the use of wrist bandages with weights, which can be useful to increase the inertia of movement and therefore reduce tremor. Daily use objects are also adapted so they are easier to grab and use.
If all these measures fail patients are candidates for thalamus surgery. This kind of surgery can be both a thalamotomy or the implantation of a thalamic stimulator. Complications are frequent (30% in thalamotomy and 10% in deep brain stimulation) and include a worsening of ataxia, dysarthria and hemiparesis. Thalamotomy is a more efficacious surgical treatment for intractable MS tremor though the higher incidence of persistent neurological deficits in patients receiving lesional surgery supports the use of deep brain stimulation as the preferred surgical strategy.
Sleep disturbance
Around half of people with MS say they experience disturbed sleep. Sleep disturbance is not regarded as a primary effect of the MS disease itself. Rather it is regarded as a secondary effect resulting from other factors that are themselves caused or exacerbated by MS, such as spasms, pain, anxiety, depression and high caffeine intake.
MS fatigue has been found to not correlate with sleep duration, but there was some correlation with insomnia and sleep quality. It may be that primary MS fatigue is unaffected by sleep characteristics, but that sleep deprivation correlates with secondary MS fatigue.
CPAP treatment in patients with MS and sleep apnea may reduce fatigue and improve the physical quality of life.
References
References
- (November 1983). "Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS)". Neurology.
- (2005). "[Aphasia and parietal syndrome as the presenting symptoms of a demyelinating disease with pseudotumoral lesions]". Revista de Neurologia.
- (June 2006). "Psychiatric onset of multiple sclerosis". Journal of the Neurological Sciences.
- (1994). "MS COSTAR: a computerized patient record adapted for clinical research purposes". Annals of Neurology.
- "Fatigue".
- "Fatigue". Multiple Sclerosis Trust.
- (August 2022). "Fatigue in multiple sclerosis: A UK MS-register based study". Multiple Sclerosis and Related Disorders.
- (June 2021). "What's in a name? That which we call ''Multiple Sclerosis Fatigue''". Multiple Sclerosis.
- (July 2023). "Thoughts on Fatigue in Multiple Sclerosis Patients". Cureus.
- (2023). "Treatment preferences in relation to fatigue of patients with relapsing multiple sclerosis: A discrete choice experiment". Multiple Sclerosis Journal: Experimental, Translational and Clinical.
- (June 2019). "Pathophysiological and cognitive mechanisms of fatigue in multiple sclerosis". Journal of Neurology, Neurosurgery, and Psychiatry.
- (September 2022). "Neurostructural and Neurophysiological Correlates of Multiple Sclerosis Physical Fatigue: Systematic Review and Meta-Analysis of Cross-Sectional Studies". Neuropsychology Review.
- (July 2016). "Central fatigue in multiple sclerosis: a review of the literature". The Journal of Spinal Cord Medicine.
- (August 2020). "Neural mechanisms underlying state mental fatigue in multiple sclerosis: a pilot study". Journal of Neurology.
- (November 2015). "Elevated body temperature is linked to fatigue in an Italian sample of relapsing-remitting multiple sclerosis patients". Journal of Neurology.
- (September 2017). "Relationship between perceived fatigue and performance fatigability in people with multiple sclerosis: A systematic review and meta-analysis". Journal of Psychosomatic Research.
- (2022). "The pathophysiology of motor fatigue and fatigability in multiple sclerosis". Frontiers in Neurology.
- "Empowering people affected by MS to live their best lives".
- "Fatigue in Patients With Multiple Sclerosis".
- "Relapsing remitting MS (RRMS)".
- (May 1, 2023). "Overview of the Current Pathophysiology of Fatigue in Multiple Sclerosis, Its Diagnosis and Treatment Options - Review Article". Neuropsychiatric Disease and Treatment.
- "Fatigue in Patients with Multiple Sclerosis".
- (2015). "Fatigue in Multiple Sclerosis: Neural Correlates and the Role of Non-Invasive Brain Stimulation". Frontiers in Cellular Neuroscience.
- (July 2019). "Importance of fatigue and its measurement in chronic liver disease". World Journal of Gastroenterology.
- (June 2013). "Fatigue". European Journal of Hospital Pharmacy.
- The Royal College of Physicians. (2004). "Multiple Sclerosis. National clinical guideline for diagnosis and management in primary and secondary care". Sarum ColourView Group.
- (June 2003). "Fatigue associated with multiple sclerosis: diagnosis, impact and management". Multiple Sclerosis.
- (2003). "Effects of treatment for depression on fatigue in multiple sclerosis". Psychosomatic Medicine.
- (June 2020). "Brain anatomical correlates of fatigue in multiple sclerosis". Multiple Sclerosis.
- (2023). "Shared imaging markers of fatigue across multiple sclerosis, aquaporin-4 antibody neuromyelitis optica spectrum disorder and MOG antibody disease". Brain Communications.
- (March 2023). "Structural and functional magnetic resonance imaging correlates of fatigue and dual-task performance in progressive multiple sclerosis". Journal of Neurology.
- (December 2018). "The neural basis of fatigue in multiple sclerosis: A multimodal MRI approach". Neurology. Clinical Practice.
- (November 2016). "Fatigue in multiple sclerosis: The contribution of occult white matter damage". Multiple Sclerosis.
- (November 2014). "Regional but not global brain damage contributes to fatigue in multiple sclerosis". Radiology.
- (February 2017). "Integrity of normal-appearing white matter: Influence of age, visible lesion burden and hypertension in patients with small-vessel disease". Journal of Cerebral Blood Flow and Metabolism.
- (March 2009). "Fatigue in multiple sclerosis is associated with the disruption of frontal and parietal pathways". Multiple Sclerosis.
- (October 1, 2024). "Fatigue in early multiple sclerosis: MRI metrics of neuroinflammation, relapse and neurodegeneration". Brain Communications.
- (January 2007). "Amantadine for fatigue in multiple sclerosis". The Cochrane Database of Systematic Reviews.
- (April 2003). "Amantadine". US National Library of Medicine.
- (August 1992). "A double-blind, randomized, crossover trial of pemoline in fatigue associated with multiple sclerosis". Neurology.
- (January 2006). "Pemoline". US National Library of Medicine.
- (2023-09-01). "Comparing Treatments for Multiple Sclerosis-Related Fatigue - Evidence Update for Clinicians {{!}} PCORI".
- (October 2005). "Randomized controlled trial of an energy conservation course for persons with multiple sclerosis". Multiple Sclerosis.
- (2007). "Use and perceived effectiveness of energy conservation strategies for managing multiple sclerosis fatigue". The American Journal of Occupational Therapy.
- (2023). "Management of multiple sclerosis fatigue in the digital age: from assessment to treatment". Frontiers in Neuroscience.
- (November 1999). "Urinary, faecal and sexual dysfunction in patients with multiple sclerosis". Journal of Neurology.
- (2000). "[Urinary alterations in multiple sclerosis]". Revista de Neurologia.
- (March 1993). "Urinary symptoms and the neurological features of bladder dysfunction in multiple sclerosis". Journal of Neurology, Neurosurgery, and Psychiatry.
- (April 2000). "Cerebral activation during micturition in normal men". Brain.
- (2002). "[Symptomatic treatment of multiple sclerosis]". Revista de Neurologia.
- "Alfuzosin". U.S. National Library of Medicine.
- "Trospium". U.S. National Library of Medicine.
- "Flavoxate". U.S. National Library of Medicine.
- (July 2005). "Efficacy of desmopressin in patients with multiple sclerosis suffering from bladder dysfunction: a meta-analysis". Acta Neurologica Scandinavica.
- (8 August 2019). "Urologic Management in Neurologic Disease: Overview, Neuroanatomy of Pelvic Floor, Neurophysiology of Pelvic Floor".
- The National Collaborating Centre for Chronic Conditions (UK). (2004). "Multiple sclerosis: national clinical guideline for diagnosis and management in primary and secondary care". Royal College of Physicians (UK).
- (2003). "Bladder, bowel and sexual dysfunction in multiple sclerosis: management strategies". Drugs.
- (June 2003). "Cognitive dysfunction in multiple sclerosis: a review of recent developments". Current Opinion in Neurology.
- (October 2001). "Cognitive dysfunction in early-onset multiple sclerosis: a reappraisal after 10 years". Archives of Neurology.
- (2018). "Recommendations for cognitive screening and management in multiple sclerosis care". Multiple Sclerosis Journal.
- (23 December 2015). "Cognitive Changes".
- (2018). "Cognition in multiple sclerosis". Neurology.
- (August 2002). "Assessing functional status: exploring the relationship between the multiple sclerosis functional composite and driving". Archives of Physical Medicine and Rehabilitation.
- (May 1991). "Cognitive dysfunction in multiple sclerosis. I. Frequency, patterns, and prediction". Neurology.
- (2023). "Managing cognitive impairment and its impact in multiple sclerosis: An Australian multidisciplinary perspective". Multiple Sclerosis and Related Disorders.
- (January 1998). "Attention impairment in recently diagnosed multiple sclerosis". European Journal of Neurology.
- (April 2003). "Cognitive impairment in probable multiple sclerosis". Journal of Neurology, Neurosurgery, and Psychiatry.
- (November 2023). "Multiple sclerosis lesions that impair memory map to a connected memory circuit". Journal of Neurology.
- (July 2004). "Correlating brain atrophy with cognitive dysfunction, mood disturbances, and personality disorder in multiple sclerosis". Journal of Neuroimaging.
- (December 2008). "Cognitive impairment in multiple sclerosis". The Lancet. Neurology.
- (March 1996). "Depression and multiple sclerosis". Neurology.
- (December 2003). "Major depression in multiple sclerosis: a population-based perspective". Neurology.
- (April 2005). "Depression in multiple sclerosis: a review". Journal of Neurology, Neurosurgery, and Psychiatry.
- (August 1991). "Cause of death in patients attending multiple sclerosis clinics". Neurology.
- Murray ED, Buttner N, Price BH. (2012) Depression and Psychosis in Neurological Practice. In: Neurology in Clinical Practice, 6th Edition. Bradley WG, Daroff RB, Fenichel GM, Jankovic J (eds.) Butterworth Heinemann. April 12, 2012. {{ISBN. 1-4377-0434-4. {{ISBN. 978-1-4377-0434-1
- (August 1994). "Treatment of abnormal eye movements that impair vision: strategies based on current concepts of physiology and pharmacology". Annals of Neurology.
- (January 1997). "Drug therapy for acquired pendular nystagmus in multiple sclerosis". Journal of Neurology.
- (June 2000). "The management of multiple sclerosis patients". Current Opinion in Neurology.
- (November 2002). "Therapeutic external ophthalmoplegia with bilateral retrobulbar botulinum toxin- an effective treatment for acquired nystagmus with oscillopsia". Eye.
- (November 2002). "Combined pharmacologic and surgical approach to acquired nystagmus due to multiple sclerosis". American Journal of Ophthalmology.
- (February 1989). "The natural history of multiple sclerosis: a geographically based study. I. Clinical course and disability". Brain.
- (April 2001). "Improving mobility and functional independence in persons with multiple sclerosis". Journal of Neurology.
- (October 1995). "What we have learned from the Optic Neuritis Treatment Trial". Ophthalmology.
- (December 2001). "The 5-year risk of MS after optic neuritis: experience of the optic neuritis treatment trial. 1997". Neurology.
- (February 2007). "Cellular mechanisms underlying the pharmacological induction of phosphenes". British Journal of Pharmacology.
- (December 2018). "Optimal Intereye Difference Thresholds in Retinal Nerve Fiber Layer Thickness for Predicting a Unilateral Optic Nerve Lesion in Multiple Sclerosis". Journal of Neuro-Ophthalmology.
- (February 2021). "Advances in ophthalmic structural and functional measures in multiple sclerosis: do the potential ocular biomarkers meet the unmet needs?". Current Opinion in Neurology.
- (February 2022). "Retinal inter-eye difference and atrophy progression in multiple sclerosis diagnostics". Journal of Neurology, Neurosurgery, and Psychiatry.
- (October 19, 2020). "Retinal layer thinning is reflecting disability progression independent of relapse activity in multiple sclerosis". Multiple Sclerosis Journal: Experimental, Translational and Clinical.
- (May 2016). "Retinal thickness measured with optical coherence tomography and risk of disability worsening in multiple sclerosis: a cohort study". The Lancet. Neurology.
- (May 2013). "Prevalence and natural history of pain in adults with multiple sclerosis: systematic review and meta-analysis". Pain.
- "VA.gov | Veterans Affairs".
- Trust, M. S.. "Pain | MS Trust".
- (September 17, 2015). "Comorbidity is associated with pain-related activity limitations in multiple sclerosis". Multiple Sclerosis and Related Disorders.
- (July 1994). "Pain prevalence, severity and impact in a clinic sample of multiple sclerosis patients". Pain.
- (November 25, 2022). "MS Hug: 7 Tips for Relieving MS Hug Symptoms". MasterHealth.
- (2002). "Pain in multiple sclerosis: a biopsychosocial perspective". Journal of Rehabilitation Research and Development.
- "Carbamazepine". U.S. National Library of Medicine.
- "Phenytoin". U.S. National Library of Medicine.
- "Gabapentin". U.S. National Library of Medicine.
- (2000). "Low-dose gabapentin combined with either lamotrigine or carbamazepine can be useful therapies for trigeminal neuralgia in multiple sclerosis". European Neurology.
- (May 1994). "Long-term results after glycerol rhizotomy for multiple sclerosis-related trigeminal neuralgia". The Canadian Journal of Neurological Sciences. Le Journal Canadien des Sciences Neurologiques.
- (December 2005). "Some patients with multiple sclerosis have neurovascular compression causing their trigeminal neuralgia and can be treated effectively with MVD: report of five cases". British Journal of Neurosurgery.
- (2003). "Microvascular decompression for trigeminal neuralgia in patients with multiple sclerosis". Stereotactic and Functional Neurosurgery.
- (August 1993). "Anatomic-radiologic basis of Lhermitte's sign in multiple sclerosis". Archives of Neurology.
- (August 2005). "Reappraisal of Lhermitte's sign in multiple sclerosis". Multiple Sclerosis.
- (April 1995). "Resolution of Lhermitte's sign in multiple sclerosis by treatment with weak electromagnetic fields". The International Journal of Neuroscience.
- (April 1982). "Lhermitte's sign in multiple sclerosis: a clinical survey and review of the literature". Journal of Neurology, Neurosurgery, and Psychiatry.
- "Clonazepam". U.S. National Library of Medicine.
- "Amitriptyline". U.S. National Library of Medicine.
- (December 1988). "Pain syndromes in multiple sclerosis". Neurology.
- (July 2017). "Olfactory dysfunction in patients with primary progressive MS". Neurology.
- (4 April 2022). "Smell test might predict DMT affectiveness".
- (April 2018). "Olfactory dysfunction in multiple sclerosis". Multiple Sclerosis and Related Disorders.
- (June 22, 2022). "Recommendations | Multiple sclerosis in adults: management | Guidance | NICE".
- Trust, M. S.. "Spasticity and spasms | MS Trust".
- "Understanding MS Spasms and Stiffness | MS Society".
- (May 2000). "Update on multiple sclerosis rehabilitation". Journal of Neurovirology.
- (December 2009). "Whole plant cannabis extracts in the treatment of spasticity in multiple sclerosis: a systematic review". BMC Neurology.
- (April 2003). "Baclofen oral". U.S. National Library of Medicine.
- (April 2003). "Dantrolene oral". U.S. National Library of Medicine.
- (April 2003). "Diazepam". U.S. National Library of Medicine.
- (April 2003). "Tizanidine". U.S. National Library of Medicine.
- (2003). "Treatments for spasticity and pain in multiple sclerosis: a systematic review". Health Technology Assessment.
- (August 2002). "Clinical effectiveness of oral treatments for spasticity in multiple sclerosis: a systematic review". Multiple Sclerosis.
- (August 1995). "Long-term intrathecal baclofen therapy in patients with intractable spasticity". The Canadian Journal of Neurological Sciences. Le Journal Canadien des Sciences Neurologiques.
- Communications, Hoff. (December 23, 2015). "Speech Difficulties".
- "Empowering people affected by MS to live their best lives".
- Trust, M. S.. "Speech problems | MS Trust".
- Richard Senelick (Reviewer). (Aug 2012). "The Speech and Swallowing Problems of Multiple Sclerosis". Web MD.
- (January 2020). "The frequency of longitudinally extensive transverse myelitis in MS: A population-based study". Multiple Sclerosis and Related Disorders.
- (February 2007). "Tremor in multiple sclerosis". Journal of Neurology.
- (January 1987). "A controlled trial of isoniazid therapy for action tremor in multiple sclerosis". Journal of Neurology.
- (December 1985). "Isoniazid for tremor in multiple sclerosis: a controlled trial". Neurology.
- (September 1985). "Controlled trial of isoniazid therapy for severe postural cerebellar tremor in multiple sclerosis". Neurology.
- (April 2003). "Isoniazid". U.S. National Library of Medicine.
- (March 1984). "Pharmacologic trials in the treatment of cerebellar tremor". Archives of Neurology.
- (August 1989). "Treatment of cerebellar tremors with carbamazepine: a controlled trial with long-term follow-up". Neurology.
- "Propranolol (Cardiovascular)". U.S. National Library of Medicine.
- (May 1991). "Glutethimide treatment of disabling action tremor in patients with multiple sclerosis and traumatic brain injury". Archives of Neurology.
- (January 2007). "Treatment for ataxia in multiple sclerosis". The Cochrane Database of Systematic Reviews.
- (July 1993). "The effect of mechanical damping loads on disabling action tremor". Neurology.
- (August 2005). "Thalamotomy versus thalamic stimulation for multiple sclerosis tremor". Journal of Clinical Neuroscience.
- "Sleep and MS | MS Trust".
- "Empowering people affected by MS to live their best lives".
- (2021). "Sleep Disorders in Relapsing-Remitting Multiple Sclerosis Patients". Wiadomości Lekarskie.
- (2006). "Sleep and fatigue in multiple sclerosis". Multiple Sclerosis Journal.
- (2022). "Poor sleep and multiple sclerosis: Associations with symptoms of multiple sclerosis and quality of life". Journal of Neurology, Neurosurgery & Psychiatry.
- (16 May 2024). "Sleep Quality in MS Impacted by Comorbidities, Study Finds".
- (2023). "Sleep disturbance and fatigue in multiple sclerosis: A systematic review and meta-analysis". Multiple Sclerosis Journal - Experimental, Translational and Clinical.
- (2015). "Fatigue in Multiple Sclerosis: A Look at the Role of Poor Sleep". Frontiers in Neurology.
- (15 November 2023). "Effects of Long-term CPAP Therapy in Multiple Sclerosis: Daria Trojan, MD, MSC".
- (November 2022). "Heat and cold sensitivity in multiple sclerosis: A patient-centred perspective on triggers, symptoms, and thermal resilience practices". Multiple Sclerosis and Related Disorders.
- (November 2010). "Thermoregulation in multiple sclerosis". Journal of Applied Physiology.
- "Temperature sensitivity".
- (July 2014). "Body temperature is elevated and linked to fatigue in relapsing-remitting multiple sclerosis, even without heat exposure". Archives of Physical Medicine and Rehabilitation.
- "Heat Sensitivity".
- Trust, M. S.. "Temperature sensitivity | MS Trust".
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Signs and symptoms of multiple sclerosis — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report