From Surf Wiki (app.surf) — the open knowledge base
Phagocyte
Cells that ingest harmful matter within the body
Cells that ingest harmful matter within the body
Phagocytes are cells that protect the body by ingesting harmful foreign particles, bacteria, and dead or dying cells. They include monocytes, macrophages, neutrophils, tissue dendritic cells, and mast cells. Their name comes from the Greek phagein, "to eat" or "devour", and "-cyte", the suffix in biology denoting "cell", from the Greek kutos, "hollow vessel". They are essential for fighting infections and for subsequent immunity. Phagocytes are important throughout the animal kingdom and are highly developed within vertebrates. One litre of human blood contains about six billion phagocytes. They were discovered in 1882 by Ilya Ilyich Mechnikov while he was studying starfish larvae. Mechnikov was awarded the 1908 Nobel Prize in Physiology or Medicine for his discovery. Phagocytes occur in many species; some amoebae behave like macrophage phagocytes, which suggests that phagocytes appeared early in the evolution of life.
Phagocytes of humans and other animals are called "professional" or "non-professional" depending on how effective they are at phagocytosis. The professional phagocytes include many types of white blood cells (such as neutrophils, monocytes, macrophages, mast cells, and dendritic cells). The main difference between professional and non-professional phagocytes is that the professional phagocytes have molecules called receptors on their surfaces that can detect harmful objects, such as bacteria, that are not normally found in the body. Non-professional phagocytes do not have efficient phagocytic receptors, such as those for opsonins. Phagocytes are crucial in fighting infections, as well as in maintaining healthy tissues by removing dead and dying cells that have reached the end of their lifespan.
During an infection, chemical signals attract phagocytes to places where the pathogen has invaded the body. These chemicals may come from bacteria or from other phagocytes already present. The phagocytes move by a method called chemotaxis. When phagocytes come into contact with bacteria, the receptors on the phagocyte's surface will bind to them. This binding will lead to the engulfing of the bacteria by the phagocyte. After phagocytosis, macrophages and dendritic cells can also participate in antigen presentation, a process in which a phagocyte moves parts of the ingested material back to its surface. This material is then displayed to other cells of the immune system. Some phagocytes then travel to the body's lymph nodes and display the material to white blood cells called lymphocytes. This process is important in building immunity, and many pathogens have evolved methods to evade attacks by phagocytes.
History

The Russian zoologist Ilya Ilyich Mechnikov (1845–1916) first recognized that specialized cells were involved in defense against microbial infections. In 1882, he studied motile (freely moving) cells in the larvae of starfishes, believing they were important to the animals' immune defenses. To test his idea, he inserted small thorns from a tangerine tree into the larvae. After a few hours, he noticed that the motile cells had surrounded the thorns. Mechnikov traveled to Vienna and shared his ideas with Carl Friedrich Claus who suggested the name "phagocyte" (from the Greek words phagein, meaning "to eat or devour", and kutos, meaning "hollow vessel") for the cells that Mechnikov had observed.
A year later, Mechnikov studied a fresh water crustacean called Daphnia, a tiny transparent animal that can be examined directly under a microscope. He discovered that fungal spores that attacked the animal were destroyed by phagocytes. He went on to extend his observations to the white blood cells of mammals and discovered that the bacterium Bacillus anthracis could be engulfed and killed by phagocytes, a process that he called phagocytosis. Mechnikov proposed that phagocytes were a primary defense against invading organisms.
In 1903, Almroth Wright discovered that phagocytosis was reinforced by specific antibodies that he called opsonins, from the Greek opson, "a dressing or relish". Mechnikov was awarded (jointly with Paul Ehrlich) the 1908 Nobel Prize in Physiology or Medicine for his work on phagocytes and phagocytosis.
Although the importance of these discoveries slowly gained acceptance during the early twentieth century, the intricate relationships between phagocytes and all the other components of the immune system were not known until the 1980s.
Phagocytosis
Main article: Phagocytosis
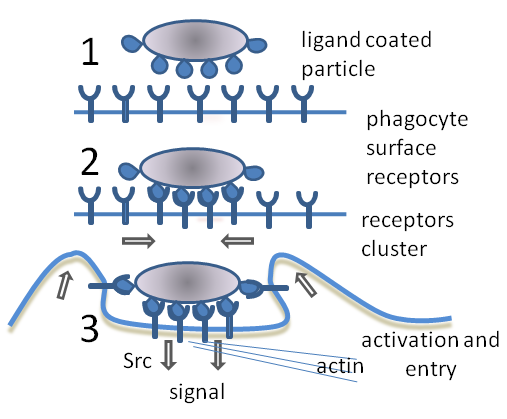
Phagocytosis is the process of taking in particles such as bacteria, invasive fungi, parasites, dead host cells, and cellular and foreign debris by a cell. It involves a chain of molecular processes. Phagocytosis occurs after the foreign body, a bacterial cell, for example, has bound to molecules called "receptors" that are on the surface of the phagocyte. The phagocyte then stretches itself around the bacterium and engulfs it. Phagocytosis of bacteria by human neutrophils takes on average nine minutes. Once inside this phagocyte, the bacterium is trapped in a compartment called a phagosome. Within one minute the phagosome merges with either a lysosome or a granule to form a phagolysosome. The bacterium is then subjected to an overwhelming array of killing mechanisms and is dead a few minutes later. Dendritic cells and macrophages are not so fast, and phagocytosis can take many hours in these cells. Macrophages are slow and untidy eaters; they engulf huge quantities of material and frequently release some undigested back into the tissues. This debris serves as a signal to recruit more phagocytes from the blood. Phagocytes have voracious appetites; scientists have even fed macrophages with iron filings and then used a small magnet to separate them from other cells.
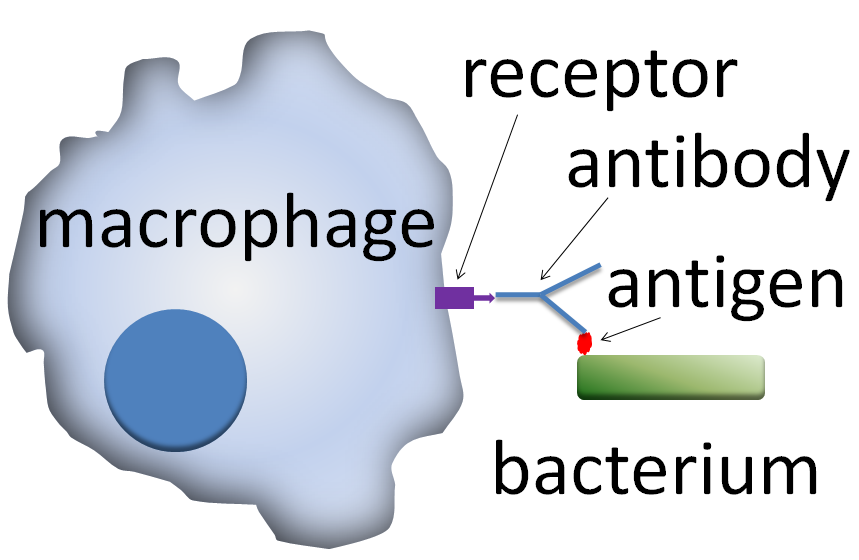
A phagocyte has many types of receptors on its surface that are used to bind material. Scavenger receptors bind to a large range of molecules on the surface of bacterial cells, and Toll-like receptors—so called because of their similarity to well-studied receptors in fruit flies that are encoded by the Toll gene—bind to more specific molecules including foreign DNA and RNA. Binding to Toll-like receptors increases phagocytosis and causes the phagocyte to release a group of hormones that cause inflammation.
Methods of killing

The killing of microbes is a critical function of phagocytes that is performed either within the phagocyte (intracellular killing) or outside of the phagocyte (extracellular killing).{{cite journal | doi-access = free }}
Oxygen-dependent intracellular
When a phagocyte ingests bacteria (or any material), its oxygen consumption increases. The increase in oxygen consumption, called a respiratory burst, produces reactive oxygen-containing molecules that are anti-microbial. The oxygen compounds are toxic to both the invader and the cell itself, so they are kept in compartments inside the cell. This method of killing invading microbes by using the reactive oxygen-containing molecules is referred to as oxygen-dependent intracellular killing, of which there are two types.
The first type is the oxygen-dependent production of a superoxide, The superoxide is converted to hydrogen peroxide and singlet oxygen by an enzyme called superoxide dismutase. Superoxides also react with the hydrogen peroxide to produce hydroxyl radicals, which assist in killing the invading microbe.
The second type involves the use of the enzyme myeloperoxidase from neutrophil granules. When granules fuse with a phagosome, myeloperoxidase is released into the phagolysosome, and this enzyme uses hydrogen peroxide and chlorine to create hypochlorite, a substance used in domestic bleach. Hypochlorite is extremely toxic to bacteria.
Oxygen-independent intracellular
Phagocytes can also kill microbes by oxygen-independent methods, but these are not as effective as the oxygen-dependent ones. There are four main types. The first uses electrically charged proteins that damage the bacterium's membrane. The second type uses lysozymes; these enzymes break down the bacterial cell wall. The third type uses lactoferrins, which are present in neutrophil granules and remove essential iron from bacteria. The fourth type uses proteases and hydrolytic enzymes; these enzymes are used to digest the proteins of destroyed bacteria.
Extracellular
Interferon-gamma—which was once called macrophage activating factor—stimulates macrophages to produce nitric oxide. The source of interferon-gamma can be CD4+ T cells, CD8+ T cells, natural killer cells, B cells, natural killer T cells, monocytes, other macrophages, or dendritic cells. Nitric oxide is then released from the macrophage and, because of its toxicity, kills microbes near the macrophage.—kills cancer cells and cells infected by viruses, and helps to activate the other cells of the immune system.
In some diseases, e.g., the rare chronic granulomatous disease, the efficiency of phagocytes is impaired, and recurrent bacterial infections are a problem.{{cite journal
Viruses
Viruses can reproduce only inside cells, and they can gain entry by using many of the receptors involved in immunity. Once inside the cell, viruses use the cell's biological machinery to their own advantage, forcing the cell to make hundreds of identical copies of themselves. Although phagocytes and other components of the innate immune system can, to a limited extent, control viruses, once a virus is inside a cell the adaptive immune responses, particularly the lymphocytes, are more important for defense. At the sites of viral infections, lymphocytes often vastly outnumber all the other cells of the immune system; this is common in viral meningitis. Virus-infected cells that have been killed by lymphocytes are cleared from the body by phagocytes.
Role in apoptosis
Main article: Apoptosis
In an animal, cells are constantly dying. A balance between cell division and cell death keeps the number of cells relatively constant in adults. There are two different ways a cell can die: by necrosis or by apoptosis. In contrast to necrosis, which often results from disease or trauma, apoptosis—or programmed cell death—is a normal healthy function of cells. The body has to rid itself of millions of dead or dying cells every day, and phagocytes play a crucial role in this process.
Dying cells that undergo the final stages of apoptosis display molecules, such as phosphatidylserine, on their cell surface to attract phagocytes.{{cite journal
Interactions with other cells
Phagocytes are usually not bound to any particular organ but move through the body interacting with the other phagocytic and non-phagocytic cells of the immune system. They can communicate with other cells by producing chemicals called cytokines, which recruit other phagocytes to the site of infections or stimulate dormant lymphocytes. Phagocytes form part of the innate immune system, which animals, including humans, are born with. Innate immunity is very effective but non-specific in that it does not discriminate between different sorts of invaders. On the other hand, the adaptive immune system of jawed vertebrates—the basis of acquired immunity—is highly specialized and can protect against almost any type of invader. The adaptive immune system is not dependent on phagocytes but lymphocytes, which produce protective proteins called antibodies, which tag invaders for destruction and prevent viruses from infecting cells. Phagocytes, in particular dendritic cells and macrophages, stimulate lymphocytes to produce antibodies by an important process called antigen presentation.
Antigen presentation
Main article: Antigen presentation
Antigen presentation is a process in which some phagocytes move parts of engulfed materials back to the surface of their cells and "present" them to other cells of the immune system. There are two "professional" antigen-presenting cells: macrophages and dendritic cells. After engulfment, foreign proteins (the antigens) are broken down into peptides inside dendritic cells and macrophages. These peptides are then bound to the cell's major histocompatibility complex (MHC) glycoproteins, which carry the peptides back to the phagocyte's surface where they can be "presented" to lymphocytes. This enhances immunity because the lymphocytes respond to the antigens presented by the dendritic cells just as they would at the site of the original infection. But dendritic cells can also destroy or pacify lymphocytes if they recognize components of the host body; this is necessary to prevent autoimmune reactions. This process is called tolerance.
Immunological tolerance
Main article: Immunological tolerance
Dendritic cells also promote immunological tolerance, which stops the body from attacking itself. The first type of tolerance is central tolerance, that occurs in the thymus. T cells that bind (via their T cell receptor) to self antigen (presented by dendritic cells on MHC molecules) too strongly are induced to die. The second type of immunological tolerance is peripheral tolerance. Some self reactive T cells escape the thymus for a number of reasons, mainly due to the lack of expression of some self antigens in the thymus. Another type of T cell; T regulatory cells can down regulate self reactive T cells in the periphery. When immunological tolerance fails, autoimmune diseases can follow.
Professional phagocytes

Phagocytes of humans and other jawed vertebrates are divided into "professional" and "non-professional" groups based on the efficiency with which they participate in phagocytosis. The professional phagocytes are myeloid cells, which includes monocytes, macrophages, neutrophils, tissue dendritic cells and mast cells. One litre of human blood contains about six billion phagocytes.
Activation
All phagocytes, and especially macrophages, exist in degrees of readiness. Macrophages are usually relatively dormant in the tissues and proliferate slowly. In this semi-resting state, they clear away dead host cells and other non-infectious debris and rarely take part in antigen presentation. But, during an infection, they receive chemical signals—usually interferon gamma—which increases their production of MHC II molecules and which prepares them for presenting antigens. In this state, macrophages are good antigen presenters and killers. If they receive a signal directly from an invader, they become "hyperactivated", stop proliferating, and concentrate on killing. Their size and rate of phagocytosis increases—some become large enough to engulf invading protozoa.
In the blood, neutrophils are inactive but are swept along at high speed. When they receive signals from macrophages at the sites of inflammation, they slow down and leave the blood. In the tissues, they are activated by cytokines and arrive at the battle scene ready to kill.
Migration
When an infection occurs, a chemical "SOS" signal is given off to attract phagocytes to the site. These chemical signals may include proteins from invading bacteria, clotting system peptides, complement products, and cytokines that have been given off by macrophages located in the tissue near the infection site.
To reach the site of infection, phagocytes leave the bloodstream and enter the affected tissues. Signals from the infection cause the endothelial cells that line the blood vessels to make a protein called selectin, which neutrophils stick to on passing by. Other signals called vasodilators loosen the junctions connecting endothelial cells, allowing the phagocytes to pass through the wall. Chemotaxis is the process by which phagocytes follow the cytokine "scent" to the infected spot. During an infection, millions of neutrophils are recruited from the blood, but they die after a few days.
Monocytes
Main article: Monocytes
Monocytes develop in the bone marrow and reach maturity in the blood. Mature monocytes have large, smooth, lobed nuclei and abundant cytoplasm that contains granules. Monocytes ingest foreign or dangerous substances and present antigens to other cells of the immune system. Monocytes form two groups: a circulating group and a marginal group that remain in other tissues (approximately 70% are in the marginal group). Most monocytes leave the blood stream after 20–40 hours to travel to tissues and organs and in doing so transform into macrophages or dendritic cells depending on the signals they receive. There are about 500 million monocytes in one litre of human blood.
Macrophages
Main article: Macrophages
Mature macrophages do not travel far but stand guard over those areas of the body that are exposed to the outside world. There they act as garbage collectors, antigen presenting cells, or ferocious killers, depending on the signals they receive. They derive from monocytes, granulocyte stem cells, or the cell division of pre-existing macrophages.{{cite journal
This type of phagocyte does not have granules but contains many lysosomes. Macrophages are found throughout the body in almost all tissues and organs (e.g., microglial cells in the brain and alveolar macrophages in the lungs), where they silently lie in wait. A macrophage's location can determine its size and appearance. Macrophages cause inflammation through the production of interleukin-1, interleukin-6, and TNF-alpha. Macrophages are usually only found in tissue and are rarely seen in blood circulation. The life-span of tissue macrophages has been estimated to range from four to fifteen days.
Macrophages can be activated to perform functions that a resting monocyte cannot. Other signals include TNF-alpha and lipopolysaccharides from bacteria. Th1 cells come from the differentiation of CD4+ T cells once they have responded to antigen in the secondary lymphoid tissues. Activated macrophages play a potent role in tumor destruction by producing TNF-alpha, IFN-gamma, nitric oxide, reactive oxygen compounds, cationic proteins, and hydrolytic enzymes.
Neutrophils
Main article: Neutrophils
Neutrophils are normally found in the bloodstream and are the most abundant type of phagocyte, constituting 50% to 60% of the total circulating white blood cells. One litre of human blood contains about five billion neutrophils, and live for only about five days.
The intra-cellular granules of the human neutrophil have long been recognized for their protein-destroying and bactericidal properties. Neutrophils can secrete products that stimulate monocytes and macrophages. Neutrophil secretions increase phagocytosis and the formation of reactive oxygen compounds involved in intracellular killing. Secretions from the primary granules of neutrophils stimulate the phagocytosis of IgG-antibody-coated bacteria. When encountering bacteria, fungi or activated platelets they produce web-like chromatin structures known as neutrophil extracellular traps (NETs). Composed mainly of DNA, NETs cause death by a process called netosis – after the pathogens are trapped in NETs they are killed by oxidative and non-oxidative mechanisms.
Dendritic cells
Main article: Dendritic cell
Dendritic cells are specialized antigen-presenting cells that have long outgrowths called dendrites, that help to engulf microbes and other invaders. Dendritic cells are present in the tissues that are in contact with the external environment, mainly the skin, the inner lining of the nose, the lungs, the stomach, and the intestines. Once activated, they mature and migrate to the lymphoid tissues where they interact with T cells and B cells to initiate and orchestrate the adaptive immune response. Mature dendritic cells activate T helper cells and cytotoxic T cells. The activated helper T cells interact with macrophages and B cells to activate them in turn. In addition, dendritic cells can influence the type of immune response produced; when they travel to the lymphoid areas where T cells are held they can activate T cells, which then differentiate into cytotoxic T cells or helper T cells.
Mast cells
Main article: Mast cell
Mast cells have Toll-like receptors and interact with dendritic cells, B cells, and T cells to help mediate adaptive immune functions. Mast cells express MHC class II molecules and can participate in antigen presentation; however, the mast cell's role in antigen presentation is not very well understood. Mast cells can consume and kill gram-negative bacteria (e.g., salmonella), and process their antigens. They specialize in processing the fimbrial proteins on the surface of bacteria, which are involved in adhesion to tissues. In addition to these functions, mast cells produce cytokines that induce an inflammatory response. This is a vital part of the destruction of microbes because the cytokines attract more phagocytes to the site of infection.
| Main location | Variety of phenotypes |
|---|---|
| Blood | neutrophils, monocytes |
| Bone marrow | macrophages, monocytes, sinusoidal cells, epithelial cells |
| Bone tissue | osteoclasts |
| Gut and intestinal Peyer's patches | macrophages |
| Connective tissue | histiocytes, macrophages, monocytes, dendritic cells |
| Liver | Kupffer cells, monocytes |
| Lung | self-replicating macrophages, monocytes, mast cells, dendritic cells |
| Lymphoid tissue | free and fixed macrophages and monocytes, dendritic cells |
| Nervous tissue | microglial cells (CD4+) |
| Spleen | free and fixed macrophages, monocytes, sinusoidal cells |
| Thymus | free and fixed macrophages and monocytes |
| Skin | resident Langerhans cells, other dendritic cells, conventional macrophages, mast cells |
Non-professional phagocytes
Dying cells and foreign organisms are consumed by cells other than the "professional" phagocytes.{{cite journal
Non-professional phagocytes are more limited than professional phagocytes in the type of particles they can take up. This is due to their lack of efficient phagocytic receptors, in particular opsonins—which are antibodies and complement attached to invaders by the immune system.
| Main location | Variety of phenotypes | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Blood, lymph and lymph nodes | Lymphocytes | ||||||||||
| Blood, lymph and lymph nodes | NK and LGL cells (large granular lymphocytes) | ||||||||||
| Blood | vauthors=Lin A, Loré K | title=Granulocytes: New Members of the Antigen-Presenting Cell Family | journal=Frontiers in Immunology | volume=8 | page=1781 | date=2017 | pmid=29321780 | pmc=5732227 | doi=10.3389/fimmu.2017.01781 | doi-access=free }} | |
| Skin | Epithelial cells | ||||||||||
| Liver | vauthors=Davies SP, Terry LV, Wilkinson AL, Stamataki Z | title=Cell-in-Cell Structures in the Liver: A Tale of Four E's | journal=Frontiers in Immunology | volume=11 | issue= | page=650 | date=2020 | pmid=32528462 | pmc=7247839 | doi=10.3389/fimmu.2020.00650 | doi-access=free }} |
| Blood vessels | Endothelial cells | ||||||||||
| Connective tissue | Fibroblasts |
Pathogen evasion and resistance

A pathogen is only successful in infecting an organism if it can get past its defenses. Pathogenic bacteria and protozoa have developed a variety of methods to resist attacks by phagocytes, and many actually survive and replicate within phagocytic cells.
Avoiding contact
There are several ways bacteria avoid contact with phagocytes. First, they can grow in sites that phagocytes are not capable of traveling to (e.g., the surface of unbroken skin). Second, bacteria can suppress the inflammatory response; without this response to infection phagocytes cannot respond adequately. Third, some species of bacteria can inhibit the ability of phagocytes to travel to the site of infection by interfering with chemotaxis. which is produced naturally by the body and plays a crucial role in wound healing.
Avoiding engulfment
Bacteria often produce capsules made of proteins or sugars that coat their cells and interfere with phagocytosis. and the exopolysaccharide capsules of Staphylococcus epidermidis. Streptococcus pneumoniae produces several types of capsule that provide different levels of protection, and group A streptococci produce proteins such as M protein and fimbrial proteins to block engulfment. Some proteins hinder opsonin-related ingestion; Staphylococcus aureus produces Protein A to block antibody receptors, which decreases the effectiveness of opsonins. Enteropathogenic species of the genus Yersinia bind with the use of the virulence factor YopH to receptors of phagocytes from which they influence the cells capability to exert phagocytosis.
Survival inside the phagocyte
Bacteria have developed ways to survive inside phagocytes, where they continue to evade the immune system.{{cite journal
Killing
Bacteria have developed several ways of killing phagocytes. These include cytolysins, which form pores in the phagocyte's cell membranes, streptolysins and leukocidins, which cause neutrophils' granules to rupture and release toxic substances, and exotoxins that reduce the supply of a phagocyte's ATP, needed for phagocytosis. After a bacterium is ingested, it may kill the phagocyte by releasing toxins that travel through the phagosome or phagolysosome membrane to target other parts of the cell.
Disruption of cell signaling
Some survival strategies often involve disrupting cytokines and other methods of cell signaling to prevent the phagocyte's responding to invasion. The protozoan parasites Toxoplasma gondii, Trypanosoma cruzi, and Leishmania infect macrophages, and each has a unique way of taming them. Some species of Leishmania alter the infected macrophage's signalling, repress the production of cytokines and microbicidal molecules—nitric oxide and reactive oxygen species—and compromise antigen presentation.{{cite journal|vauthors=Gregory DJ, Olivier M| title = Subversion of host cell signalling by the protozoan parasite Leishmania| journal = Parasitology| volume = 130 Suppl| pages = S27–35| year = 2005| pmid = 16281989| doi = 10.1017/S0031182005008139
Host damage by phagocytes
Macrophages and neutrophils, in particular, play a central role in the inflammatory process by releasing proteins and small-molecule inflammatory mediators that control infection but can damage host tissue. In general, phagocytes aim to destroy pathogens by engulfing them and subjecting them to a battery of toxic chemicals inside a phagolysosome. If a phagocyte fails to engulf its target, these toxic agents can be released into the environment (an action referred to as "frustrated phagocytosis"). As these agents are also toxic to host cells, they can cause extensive damage to healthy cells and tissues.
When neutrophils release their granule contents in the kidney, the contents of the granule (reactive oxygen compounds and proteases) degrade the extracellular matrix of host cells and can cause damage to glomerular cells, affecting their ability to filter blood and causing changes in shape. In addition, phospholipase products (e.g., leukotrienes) intensify the damage. This release of substances promotes chemotaxis of more neutrophils to the site of infection, and glomerular cells can be damaged further by the adhesion molecules during the migration of neutrophils. The injury done to the glomerular cells can cause kidney failure.
Neutrophils also play a key role in the development of most forms of acute lung injury. Here, activated neutrophils release the contents of their toxic granules into the lung environment. Experiments have shown that a reduction in the number of neutrophils lessens the effects of acute lung injury, but treatment by inhibiting neutrophils is not clinically realistic, as it would leave the host vulnerable to infection. In the liver, damage by neutrophils can contribute to dysfunction and injury in response to the release of endotoxins produced by bacteria, sepsis, trauma, alcoholic hepatitis, ischemia, and hypovolemic shock resulting from acute hemorrhage.
Chemicals released by macrophages can also damage host tissue. TNF-α is an important chemical that is released by macrophages that causes the blood in small vessels to clot to prevent an infection from spreading. If a bacterial infection spreads to the blood, TNF-α is released into vital organs, which can cause vasodilation and a decrease in plasma volume; these in turn can be followed by septic shock. During septic shock, TNF-α release causes a blockage of the small vessels that supply blood to the vital organs, and the organs may fail. Septic shock can lead to death.
Evolutionary origins
Phagocytosis is common and probably appeared early in evolution, evolving first in unicellular eukaryotes. Amoebae are unicellular protists that separated from the tree leading to metazoa shortly after the divergence of plants, and they share many specific functions with mammalian phagocytic cells. Dictyostelium discoideum, for example, is an amoeba that lives in the soil and feeds on bacteria. Like animal phagocytes, it engulfs bacteria by phagocytosis mainly through Toll-like receptors, and it has other biological functions in common with macrophages. Dictyostelium discoideum is social; it aggregates when starved to form a migrating pseudoplasmodium or slug. This multicellular organism eventually will produce a fruiting body with spores that are resistant to environmental dangers. Before the formation of fruiting bodies, the cells will migrate as a slug-like organism for several days. During this time, exposure to toxins or bacterial pathogens has the potential to compromise survival of the species by limiting spore production. Some of the amoebae engulf bacteria and absorb toxins while circulating within the slug, and these amoebae eventually die. They are genetically identical to the other amoebae in the slug; their self-sacrifice to protect the other amoebae from bacteria is similar to the self-sacrifice of phagocytes seen in the immune system of higher vertebrates. This ancient immune function in social amoebae suggests an evolutionarily conserved cellular foraging mechanism that might have been adapted to defense functions well before the diversification of amoebae into higher forms.{{cite journal
References
Bibliography
References
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Hoffbrand. Pettit. Moss. 2005
- [http://nobelprize.org/nobel_prizes/medicine/laureates/1908/mechnikov-bio.html Ilya Mechnikov], retrieved on November 28, 2008. From [http://nobelprize.org/nobelfoundation/publications/lectures/index.html Nobel Lectures], ''Physiology or Medicine 1901–1921'', Elsevier Publishing Company, Amsterdam, 1967. {{webarchive. link. (August 22, 2008)
- Schmalstieg, FC. (2008). "Ilya Ilich Metchnikoff (1845–1915) and Paul Ehrlich (1854–1915): the centennial of the 1908 Nobel Prize in Physiology or Medicine". Journal of Medical Biography.
- Janeway, Chapter: [https://www.ncbi.nlm.nih.gov/books/NBK27138/ Evolution of the innate immune system.] retrieved on March 20, 2009
- {{Harvnb. Ernst. Stendahl. 2006
- {{Harvnb. Robinson. Babcock. 1998. Ernst. Stendahl. 2006
- {{Harvnb. Ernst. Stendahl. 2006
- (October 2004). "Antimicrobial reactive oxygen and nitrogen species: concepts and controversies". Nat. Rev. Microbiol..
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- (2019). "Immunology's Coming of Age". Frontiers in Immunology.
- (1983). "The Shorter Oxford English Dictionary". Oxford University Press (Guild Publishing).
- (April 1, 1998). "Medals, memoirs—and Metchnikoff". J. Leukoc. Biol..
- "Ilya Mechnikov". The Nobel Foundation.
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Robinson. Babcock. 1998
- {{harvnb. Ernst. Stendahl. 2006
- {{Harvnb. Ernst. Stendahl. 2006
- {{Harvnb. Ernst. Stendahl. 2006
- (May 2019). "It takes a village: Phagocytes play a central role in fungal immunity". Seminars in Cell & Developmental Biology.
- (February 1994). "A single assay for measuring the rates of phagocytosis and bacterial killing by neutrophils". J. Leukoc. Biol..
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Sompayrac. 2019
- They include [[opsonin]] receptors, [[scavenger receptor (immunology). scavenger receptor]]s, and [[Toll-like receptors]]. Opsonin receptors increase the phagocytosis of bacteria that have been coated with [[immunoglobulin G]] (IgG) [[antibodies]] or with [[complement system. complement]]. "Complement" is the name given to a complex series of protein molecules found in the blood that destroy cells or mark them for destruction.{{Harvnb. Sompayrac. 2019
- (January 2019). "RNA Modifications Modulate Activation of Innate Toll-Like Receptors". Genes.
- Dahlgren, C. (December 17, 1999). "Respiratory burst in human neutrophils". Journal of Immunological Methods.
- (1999). "Myeloperoxidase". Proc. Assoc. Am. Physicians.
- {{Harvnb. Hoffbrand. Pettit. Moss. 2005
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- (February 2004). "Interferon-gamma: an overview of signals, mechanisms and functions". J. Leukoc. Biol..
- {{Harvnb. Sompayrac. 2019
- (January 2008). "Chediak-Higashi syndrome". Curr. Opin. Hematol..
- {{Harvnb. Sompayrac. 2019
- (October 2007). "Laboratorial diagnosis of lymphocytic meningitis". Braz J Infect Dis.
- {{Harvnb. Sompayrac. 2019
- (1995). "Apoptosis in the pathogenesis and treatment of disease". Science.
- {{Harvnb. Sompayrac. 2019
- "Apoptosis". Merriam-Webster Online Dictionary.
- (December 2019). "Flippase and scramblase for phosphatidylserine exposure". Current Opinion in Immunology.
- (2003). "Cell corpse engulfment mediated by ''C. elegans'' phosphatidylserine receptor through CED-5 and CED-12". Science.
- (2003). "Eat me or die". Science.
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- (2004). "Antigen Presenting Cells (APC)".
- Mature macrophages do not travel far from the site of infection, but dendritic cells can reach the body's [[lymph node]]s, where there are millions of lymphocytes.{{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- (2007). "Dendritic cell-regulatory T-cell interactions control self-directed immunity". Immunol. Cell Biol..
- Steinman, Ralph M.. (2004). "Dendritic Cells and Immune Tolerance". The Rockefeller University.
- Romagnani, S. (2006). "Immunological tolerance and autoimmunity". Internal and Emergency Medicine.
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Sompayrac. 2019
- {{Harvnb. Hoffbrand. Pettit. Moss. 2005
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- (September 1997). "Cell size of alveolar macrophages: an interspecies comparison". Environ. Health Perspect..
- {{Harvnb. Delves. Martin. Burton. Roit. 2006
- {{Harvnb. Ernst. Stendahl. 2006
- [[T helper cell]]s (also known as effector T cells or Th cells), a sub-group of lymphocytes, are responsible for the activation of macrophages. Th1 cells activate macrophages by signaling with [[IFN-gamma]] and displaying the protein [[CD40 ligand]].{{Harvnb. Delves. Martin. Burton. Roit. 2006
- Stvrtinová, Viera. (1995). "Inflammation and Fever from Pathophysiology: Principles of Disease". Academic Electronic Press.
- which are about 10 micrometers in diameter{{Harvnb. Delves. Martin. Burton. Roit. 2006
- (December 1998). "Passive deformability of mature, immature, and active neutrophils in healthy and septicemic neonates". Pediatr. Res..
- {{Harvnb. Paoletti. Notario. Ricevuti. 1997
- (January 2008). "Neutrophil secretion products regulate anti-bacterial activity in monocytes and macrophages". Clin. Exp. Immunol..
- (October 2008). "Neutrophil primary granule proteins HBP and HNP1-3 boost bacterial phagocytosis by human and murine macrophages". J. Clin. Invest..
- (February 2018). "Neutrophil extracellular traps in immunity and disease". Nature Reviews. Immunology.
- (1973). "Identification of a novel cell type in peripheral lymphoid organs of mice. I. Morphology, quantitation, tissue distribution". J. Exp. Med..
- Steinman, Ralph. "Dendritic Cells". The Rockefeller University.
- (2002). "Antigen presentation and T cell stimulation by dendritic cells". Annu. Rev. Immunol..
- {{Harvnb. Hoffbrand. Pettit. Moss. 2005
- (2002). "The instructive role of dendritic cells on T-cell responses". Arthritis Res..
- {{Harvnb. Sompayrac. 2019
- (2010). "The immunoglobulin E-Toll-like receptor network". International Archives of Allergy and Immunology.
- (November 2008). "New developments in mast cell biology". Nature Immunology.
- (February 2001). "Mast cell modulation of immune responses to bacteria". Immunol. Rev..
- (September 1996). "Type 1 fimbrial expression enhances ''Escherichia coli'' virulence for the urinary tract". Proc. Natl. Acad. Sci. U.S.A..
- (February 1996). "Mast cells process bacterial Ags through a phagocytic route for class I MHC presentation to T cells". J. Immunol..
- (2001). "Mast cells in allergy and host defense". Allergy Asthma Proc.
- (2012). "The role of mast cells in the defence against pathogens". PLOS Pathogens.
- {{Harvnb. Paoletti. Notario. Ricevuti. 1997
- (January 2001). "Involvement of actin filaments and integrins in the binding step in collagen phagocytosis by human fibroblasts". Journal of Cell Science.
- (March 1995). "Professional and non-professional phagocytes: an introduction". Trends Cell Biol..
- (2017). "Granulocytes: New Members of the Antigen-Presenting Cell Family". Frontiers in Immunology.
- (2020). "Cell-in-Cell Structures in the Liver: A Tale of Four E's". Frontiers in Immunology.
- Todar, Kenneth. "Mechanisms of Bacterial Pathogenicity: Bacterial Defense Against Phagocytes". 2008.
- (September 1999). "Leishmania species: models of intracellular parasitism". J. Cell Sci..
- (May 2002). "Bacterial avoidance of phagocytosis". Trends Microbiol..
- (September 2005). "Fibronectin fragmentation promotes alpha4beta1 integrin-mediated contraction of a fibrin-fibronectin provisional matrix". Experimental Cell Research.
- (December 2004). "A crucial role for exopolysaccharide modification in bacterial biofilm formation, immune evasion, and virulence". J. Biol. Chem..
- (February 2009). "''Streptococcus pneumoniae'' capsular serotype 19F is more resistant to C3 deposition and less sensitive to opsonophagocytosis than serotype 6B". Infect. Immun..
- (December 2005). "Immune evasion by staphylococci". Nat. Rev. Microbiol..
- (February 2002). "Resistance to phagocytosis by Yersinia". International Journal of Medical Microbiology.
- (July 2008). "Intracellular survival of ''Staphylococcus aureus'': correlating production of catalase and superoxide dismutase with levels of inflammatory cytokines". Inflamm. Res..
- (August 2007). "Cytolysin-dependent escape of the bacterium from the phagosome is required but not sufficient for induction of the Th1 immune response against Listeria monocytogenes infection: distinct role of Listeriolysin O determined by cytolysin gene replacement". Infect. Immun..
- (2021). "Antimicrobial Activity of Neutrophils Against Mycobacteria". Frontiers in Immunology.
- (May 2005). "Mutational analysis of the group A streptococcal operon encoding streptolysin S and its virulence role in invasive infection". Mol. Microbiol..
- (June 2006). "Staphylococcal cutaneous infections: invasion, evasion and aggression". J. Dermatol. Sci..
- (January 2005). "Sabotage and exploitation in macrophages parasitized by intracellular protozoans". Trends Parasitol..
- Paoletti pp. 426–30
- (August 1999). "Neutrophils and renal failure". Am. J. Kidney Dis..
- (February 2001). "Neutrophil activation and acute lung injury". Curr Opin Crit Care.
- (January 2006). "Neutrophil granule contents in the pathogenesis of lung injury". Curr. Opin. Hematol..
- (April 2003). "Neutrophils and acute lung injury". Crit. Care Med..
- (December 1997). "Host tissue damage by phagocytes". Ann. N. Y. Acad. Sci..
- (October 2006). "Porcine innate and adaptative immune responses to influenza and coronavirus infections". Ann. N. Y. Acad. Sci..
- (June 2008). "Eat, kill or die: when amoeba meets bacteria". Curr. Opin. Microbiol..
- (2008). "International Review of Cell and Molecular Biology".
- from marine sponges to insects and lower and higher vertebrates.{{Harvnb. Delves. Martin. Burton. Roit. 2006
- (April 2009). "Development of macrophages of cyprinid fish". Dev. Comp. Immunol..
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Phagocyte — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report