From Surf Wiki (app.surf) — the open knowledge base
Management of acute coronary syndrome

| Field | Value |
|---|---|
| name | Management of acute coronary syndrome |
| image | Heart attack-NIH.gif |
| caption | Acute coronary syndromes are commonly caused by a blood clot forming on an atherosclerotic plaque in a coronary artery. Oxygen delivery to a part of heart muscle is blocked, eventually causing cell death. |
| specialty | cardiology |
Management of acute coronary syndrome is targeted against the effects of reduced blood flow to the affected area of the heart muscle, usually because of a blood clot in one of the coronary arteries, the vessels that supply oxygenated blood to the myocardium. This is achieved with urgent hospitalization and medical therapy, including drugs that relieve chest pain and reduce the size of the infarct, and drugs that inhibit clot formation; for a subset of patients invasive measures are also employed (coronary angiography and percutaneous coronary intervention). Basic principles of management are the same for all types of acute coronary syndrome. However, some important aspects of treatment depend on the presence or absence of elevation of the ST segment on the electrocardiogram, which classifies cases upon presentation to either ST segment elevation myocardial infarction (STEMI) or non-ST elevation acute coronary syndrome (NST-ACS); the latter includes unstable angina and non-ST elevation myocardial infarction (NSTEMI). Treatment is generally more aggressive for STEMI patients, and reperfusion therapy is more often reserved for them. Long-term therapy is necessary for prevention of recurrent events and complications.
General principles
Acute coronary syndromes are caused by sudden and critical reduction of blood flow in one of the coronary arteries, the vessels that supply oxygenated blood to the myocardium (heart muscle), typically by a blood clot. The principal symptom is typically chest pain, known as angina pectoris; people who present with angina must prompt evaluation for possible acute coronary syndrome.
Acute coronary syndromes are classified to two major categories, according to the patient's electrocardiogram, and specifically the presence or absence of persistent (20 min) ST segment elevation (or left bundle branch block). Patients with acute coronary syndrome and ST elevation are said to have ST-elevation myocardial infarction (STEMI) and they tend to have one of their coronary arteries totally blocked. Damage is reversible for approximately 20-30 minutes after complete obstruction of blood flow; thereafter myocardial cell death ensues and progresses as time passes. Therefore, complete and sustained restoration of blood flow must be as prompt as possible to ensure maximum salvage of functional myocardium, a principle expressed in the maxim "time is muscle".See:
- This is achieved with reperfusion therapy, which is based on invasive reopening of the affected coronary artery with primary percutaneous coronary intervention, or non-invasive breaking up of the responsible blood clot with a thrombolytic drug.
Patients without ST segment elevation are said to have non-ST-elevation acute coronary syndrome and tend not to have full occlusion of a coronary artery. If there is evidence of myocardial cell death (especially elevated cardiac biomarkers) they are considered to have a non-ST-elevation myocardial infarction (NSTEMI); otherwise they are classified with unstable angina. Their management is based on the estimation of their risk for adverse events. Patients at low risk can be adequately treated with medical therapy, in many ways similar to the one used for STEMI (but excluding thrombolytics). Those at moderate to high risk benefit from an early invasive strategy, which includes coronary angiography and, if necessary, revascularization with percutaneous coronary intervention or coronary artery bypass surgery.
Medical therapy for acute coronary syndromes is based on drugs that act against ischemia and resultant angina and limit the infarct size (i.e., the area of myocardium that is affected), as well as drugs that inhibit clot formation. The latter include antiplatelet agents, which block the activation and aggregation of platelets (cellular blood components that contribute to clot formation), and anticoagulant agents (which attenuate the coagulation cascade). Long-term therapy in acute coronary syndrome survivors is targeted against recurrence and long-term complications (secondary prevention).
Women are taken less seriously than men when they have a heart attack leading to higher mortality among women.
Patient-dependent initial measures

Patients with known coronary artery disease who have been prescribed nitroglycerin should promptly take one dose, and call emergency medical services if their symptoms do not improve within 2–5 minutes. Chewing non−enteric-coated aspirin is encouraged (unless there are contraindications).
Patients should stay calmed in a comfortable position. In case of heart attack, it would not usually be lying down, but sitting down or sitting down with folded knees (but patients would notice the position that fits for them).
Patients should not be transported to hospital by private vehicles instead of an ambulance, unless evacuation by land or air ambulance is impossible (e.g., dangerous weather in a very remote area), and if they must be, it should be done if possible with someone trained in cardiac first aid.
Health care professionals are responsible for teaching their patients at risk of acute coronary syndrome what the symptoms of this condition are, and that it is imperative to seek urgent medical attention in case they present.
Emergency services
Emergency Medical Services (EMS) Systems vary considerably in their ability to evaluate and treat patients with suspected acute myocardial infarction. Some provide as little as first aid and early defibrillation. Others employ highly trained paramedics with sophisticated technology and advanced protocols. Paramedic services are capable of providing oxygen, IV access, sublingual nitroglycerine, morphine, and aspirin. Some advanced paramedic systems can also perform 12-lead ECGs. If a STEMI is recognized the paramedic may be able to contact the local PCI hospital and alert the emergency room physician, and staff of the suspected AMI. Some Paramedic services are capable of providing thrombolytic therapy in the prehospital setting, allowing reperfusion of the myocardium.
With primary PCI emerging as the preferred therapy for ST-segment elevation myocardial infarction, EMS can play a key role in reducing door-to-balloon intervals (the time from presentation to a hospital ER to the restoration of coronary artery blood flow) by performing a 12-lead ECG in the field and using this information to triage the patient to the most appropriate medical facility. In addition, the 12-lead ECG can be transmitted to the receiving hospital, which enables time saving decisions to be made prior to the arrival of the patient. This may include a "cardiac alert" or "STEMI alert" that calls in off duty personnel in areas where the cardiac cath lab is not staffed 24 hours a day. Even in the absence of a formal alerting program, prehospital 12-lead ECGs are independently associated with reduced door to treatment intervals in the emergency department.
Initial diagnostic approach
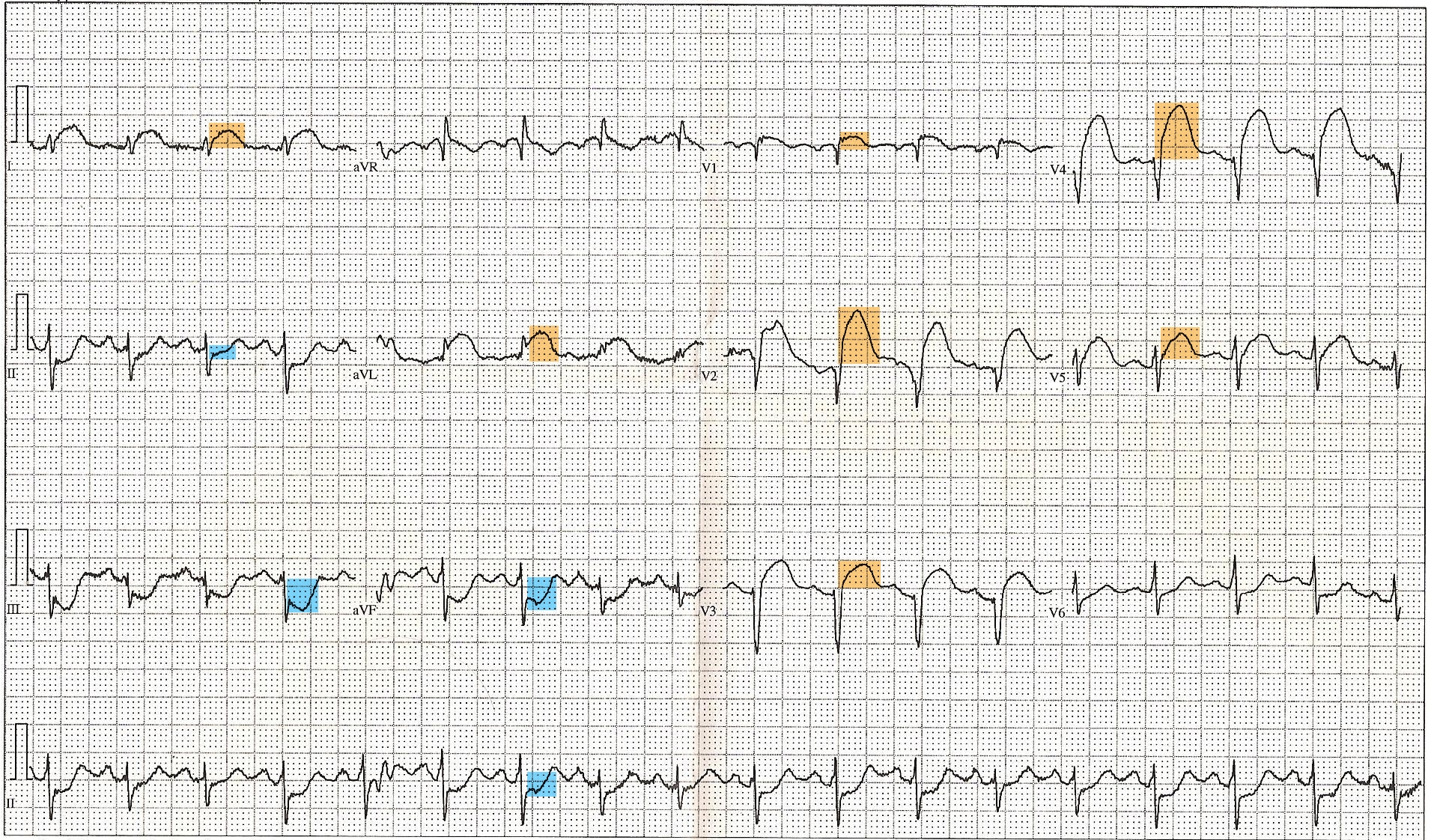
Relief of angina
Relief of the pain of angina is of paramount importance, not only for humane reasons but because the pain is associated with sympathetic activation that causes vasoconstriction and increases the workload of the heart. The pain of myocardial ischemia is likely to respond to any intervention that improves the relationship between oxygen demand and supply, like nitrates, beta blockers and oxygen.
Nitrates
Nitrates, like nitroglycerin, dilate blood vessels, which is beneficial against myocardial ischemia in two ways: By increasing blood flow in the coronary arteries and the amount of oxygen that arrives to heart muscle; and by relaxing all blood vessels in the body, thereby reducing the workload that heart needs to produce against them and the oxygen it consumes. The preferred mode of administration is sublingually. By relaxing blood vessels nitrates also reduce blood pressure, which must be carefully monitored; they must not be used if hypotension is present. They must also be avoided in patients who have taken sildenafil or other phosphodiesterase type 5 inhibitors (used for erectile dysfunction) within the previous 24–48 hours, as the combination of the two could cause a serious drop in blood pressure. Intravenous nitrates are useful in patients with hypertension or pulmonary edema.
Beta blockers
By reducing sympathetic stimulation of the heart, beta blockers decrease heart rate, blood pressure and cardiac output, and hence heart oxygen consumption. Beta-blockers alleviate ischemic pain, and have also been proved to reduce the size of infarcted heart muscle, the risk of arrhythmias, and the proportion of patients with acute coronary syndrome who actually evolve STEMI. However, they have also been shown to increase the risk of acute heart failure. Their early use is contraindicated if there are signs of congestive heart failure (e.g., Killip class II or above) or hypotension, along with other contraindications to beta blockers (slow heart rate, atrioventricular block); in the absence of contraindications beta blocker therapy should begin in the first 24 hours. It may be prudent to prefer oral rather than intravenous forms.See:
Oxygen therapy
Initial administration of oxygen to all patients with acute coronary syndrome is common practice; however, there is no evidence to support or refute that supplemental oxygen might be harmful or beneficial for cardiac patients who do not need it. It is currently recommended to give oxygen only to breathless patients or when blood oxygen saturation is low, e.g.
Analgesics
Analgesic agents that are most commonly used are opioids, and especially morphine, which is considered the analgesic of choice in patients with ST elevation. Along with its pain-controlling properties, morphine also reduces the work of breathing, alleviates breathlessness, reduces anxiety and has favorable action on hemodynamic parameters and cardiac oxygen consumption. However, in patients presenting without ST elevation, morphine has been shown to have adverse events potential, and its use is considered acceptable only after inadequate pain relief by medication specific against angina. Non-steroidal anti-inflammatory drugs are contraindicated for both categories of patients.
Antiplatelet drugs
All patients with acute coronary syndrome must immediately receive antiplatelet therapy, including aspirin and generally a second oral antiplatelet agent. Bleeding is the most important side-effect of antiplatelets.
Aspirin
Aspirin inhibits platelet aggregation and formation of blood clots. It is effective across the entire spectrum of acute coronary syndromes; it has been shown to reduce the rate of death in patients with STEMI and in patients presenting without ST elevation. Aspirin is contraindicated in patients with documented allergy or known platelet disorder. Patients who have had gastrointestinal symptoms while on long-term aspirin therapy are usually able to tolerate aspirin in the short term. For patients with true intolerance to aspirin clopidogrel is recommended. Lower doses need days to achieve full antiplatelet effect, therefore a loading dose is necessary for patients who are not already on aspirin.See:
P2Y12 inhibitors
Aside from aspirin, three antiplatelet agents taken by mouth have been approved for use in acute coronary syndromes, clopidogrel, ticagrelor and prasugrel; all reduce platelet aggregation by inhibiting the P2Y12 receptor, a type of adenosine phosphate receptor, on the surface of platelets. Not all three of them are equally indicated in all types of acute coronary syndromes. In patients with ST elevation the choice of P2Y12 inhibitor depends on reperfusion strategy; for patients undergoing primary percutaneous coronary intervention ticagrelor and prasugrel are considered superior to clopidogrel, as they are more potent and have more rapid onset of action, at the cost of some increase in bleeding risk; for STEMI patients who are treated with fibrinolysis and those who do not undergo reperfusion treatment only clopidogrel is indicated. Prasugrel must not be given to patients with a history of ischemic stroke or aged 75 years or older. In patients with non-ST elevation acute coronary syndrome current guidelines also recommend immediate administration of dual antiplatelet therapy upon diagnosis; clopidogrel and ticagrelor are indicated in this setting, with ticagrelor considered superior for patients undergoing early invasive strategy (see later). However, emerging evidence questions this strategy. As with aspirin, it is necessary to administer a loading dose.
Glycoprotein IIb/IIIa inhibitors
Glycoprotein IIb/IIIa inhibitors are a class of intravenous antiplatelet agents used in patients undergoing percutaneous coronary intervention, consisting of abciximab, eptifibatide and tirofiban. Patients presenting with ST elevation that will be reperfused with percutaneous coronary intervention may receive one of the above agents at the time of catheterization, or perhaps before. Administering eptifibatide or tirofiban may also be reasonable in patients presenting with NST-ACS who are considered of intermediate or high risk and are treated with early invasive strategy.
Antiplatelet agents
Aspirin is useful not only for the primary prevention of vascular events but is also effective across the entire spectrum of acute coronary syndromes and forms part of the initial management strategy for patients with suspected STEMI. Aspirin has been shown to markedly reduce mortality and thus should be taken as soon as possible in those without an allergy to it. Aspirin has an antiplatelet effect which inhibits formation of further thrombi (blood clots) that clog arteries. Chewing is the preferred method of administration, so that it can be absorbed quickly. Dissolved soluble preparations or sublingual administration can also be used. Because low doses take several days to achieve full antiplatelet effect, U.S. guidelines recommend a dose of 162–325 mg. Australian guidelines recommend a dose of 150–300 mg. Additionally, the antiplatelet agent clopidogrel improves outcomes in those who will be conservatively managed or undergo percutaneous coronary intervention. It however may worsen outcomes in those who need urgent coronary artery bypass surgery. --
Anticoagulants
Anticoagulants in acute coronary syndrome are targeted against the coronary blood clot, as well as towards prevention of thrombotic complications, like formation of blood clots in the ventricles, stroke, pulmonary embolism or deep vein thrombosis. Patients undergoing PCI also need an anticoagulant to prevent catheter thrombosis. Options include unfractionated heparin, enoxaparin (a low molecular weight heparin), fondaparinux (a pentasaccharide antagonist of factor Xa) and bivalirudin (a direct thrombin inhibitor); all the above agents are given parenterally (subcutaneously or intravenously). Unfractionated heparin has the disadvantage of requiring dose adjustment based on a laboratory exam, activated partial thromboplastin time (APTT). In STEMI patients choice depends on the reperfusion strategy used (see below); bivalirudin is used when PCI is employed only, while in the same case fondaparinux is not preferred. Similarly, in Non-STE ACS bivalirudin too is only used when an early invasive strategy is chosen.
Reperfusion
Main article: Reperfusion therapy
Individuals without ST segment elevation are presumed to be experiencing either unstable angina (UA) or non-ST segment elevation myocardial infarction (NSTEMI). They receive many of the same initial therapies and are often stabilized with antiplatelet drugs and anticoagulated. If their condition remains (hemodynamically) stable, they can be offered either late coronary angiography with subsequent restoration of blood flow (revascularization), or non-invasive stress testing to determine if there is significant ischemia that would benefit from revascularization. If hemodynamic instability develops in individuals with NSTEMIs, they may undergo urgent coronary angiography and subsequent revascularization. The use of thrombolytic agents is contraindicated in this patient subset, however.
The basis for this distinction in treatment regimens is that ST segment elevations on an ECG are typically due to complete occlusion of a coronary artery. On the other hand, in NSTEMIs there is typically a sudden narrowing of a coronary artery with preserved (but diminished) flow to the distal myocardium. Anticoagulation and antiplatelet agents are given to prevent the narrowed artery from occluding.
At least 10% of patients with STEMI do not develop myocardial necrosis (as evidenced by a rise in cardiac markers) and subsequent Q waves on EKG after reperfusion therapy. Such a successful restoration of flow to the infarct-related artery during an acute myocardial infarction is known as "aborting" the myocardial infarction. If treated within the hour, about 25% of STEMIs can be aborted.
Rehabilitation
Additional objectives are to prevent life-threatening arrhythmias or conduction disturbances. This requires monitoring in a coronary care unit and protocolized administration of antiarrhythmic agents. Antiarrhythmic agents are typically only given to individuals with life-threatening arrhythmias after a myocardial infarction and not to suppress the ventricular ectopy that is often seen after a myocardial infarction.
Cardiac rehabilitation aims to optimize function and quality of life in those affected by a heart disease. This can be with the help of a physician, or in the form of a cardiac rehabilitation program.
Physical exercise is an important part of rehabilitation after a myocardial infarction, with beneficial effects on cholesterol levels, blood pressure, weight, stress and mood. Patients are encouraged to exercise, and should only avoid certain exerting activities. Local authorities may place limitations on driving motor vehicles. In most cases, the advice is a gradual increase in physical exercise during about 6–8 weeks following an MI.
Some people are afraid to have sex after a heart attack. Most people can resume sexual activities after 3 to 4 weeks. The amount of activity needs to be dosed to the patient's possibilities.
Special cases
Cocaine
Cocaine associated myocardial infarction should be managed in a manner similar to other patients with acute coronary syndrome, except that beta blockers should not be used and benzodiazepines should be administered early. The treatment itself may have complications. If attempts to restore the blood flow are initiated after a critical period of only a few hours, the result may be a reperfusion injury instead of amelioration.
Wilderness setting
In wilderness first aid, a possible heart attack justifies evacuation by the fastest available means, often meaning the initiation of a MEDEVAC. The suspicion or provisional diagnosis of an MI means that it is inappropriate for the patient to walk out of the wilderness setting and will require them to be carried or conveyed in a vehicle. Aspirin, nitroglycerin, and oxygen can all be given with relative ease in a wilderness setting and should be administered as soon as possible in suspected cases of MI. Wilderness management of cardiac arrest differs slightly from that carried out in an urban setting in that it is generally considered acceptable to terminate a resuscitation attempt after 30 minutes if there has been no change in the patient's condition.
Air travel
Certified personnel traveling by commercial aircraft may be able to assist an MI patient by using the on-board first aid kit, which may contain some cardiac drugs (such as glyceryl trinitrate spray, aspirin, or opioid painkillers), an AED, and oxygen. Pilots may divert the flight to land at a nearby airport. Cardiac monitors are being introduced by some airlines, and they can be used by both on-board and ground-based physicians.
References
Selected cited works
Nitroglycerin
Nitroglycerin is used in the treatment of ACS/IHD to relieve anginal symptoms. It is associated with the decrease in myocardial stress due to peripheral vasodilation. The decrease of stress also decreases oxygen demand of the heart. The first line treatment for symptomatic relief of angina is sub-lingual nitroglycerin. Other formulations such as spray and IV can also be used. In the body nitroglycerin donates three nitric oxide molecules, which activate a second messenger system leading to release of calcium ions. The release of calcium ions leads to a relaxation of vascular smooth muscles and vasodilation. Nitroglycerin should not be given if any phosphodiesterase type 5 inhibitors such as Viagra, Cialis, Stondra, and Levitra have been taken by the casualty within the previous 24–48 hours as the combination of the two could cause a serious drop in blood pressure. It should not be given to patients with systolic blood pressure (SBP) less than 90mmHg or 30mmHg or more below baseline.
Beta Blockers
In theory β-blockers decrease the effect of the sympathetic nervous system on the heart. Since it is known that the sympathetic nervous system increases the heart rate and blood pressure in order to increase the cardiac output. Hence its blockage spares the heart the extra work load. So, the immediate intravenous administration of beta blockers reduces cardiac index, heart rate and blood pressure. Favorable effects are reduction in chest pain, in the proportion of patients with threatened infarction who actually evolve STEMI and in the development of ventricular arrhythmias. It is reasonable to administer iv beta blockers promptly to STEMI patients, especially if a tachyarrhythmia or hypertension is present, in the absence of signs of heart failure or low output, increased risk of developing shock or other relative contraindications to beta blockers.--
References
- Current management of acute coronary syndrome is based on [[medical guideline. guidelines]], produced by national and international medical societies according to the principles of [[evidence-based medicine]]. Examples are the guidelines of the [[American Heart Association]] and [[American College of Cardiology]] ({{harvnb. O'Gara. 2013, {{harvnb. Amsterdam. 2014) and those of the [[European Society of Cardiology]] ({{harvnb. Steg. 2012, {{harvnb. Hamm. 2011).
- Antman, EM. (2012a). "Braunwald's heart disease: A textbook of cardiovascular medicine". Saunders.
- Canty, JM Jr.. (2012). "Braunwald's heart disease: A textbook of cardiovascular medicine". Saunders.
- Schoen, FJ. (2010). "Robbins and Cotran pathologic basis of disease.". Saunders.
- [https://www.bbc.co.uk/news/health-42590013 Heart attack care dangerously unequal for women, study finds] ''[[BBC]]''
- (2001). "Timing is everything. Motivating patients to call 9-1-1 at onset of acute myocardial infarction". Circulation.
- "What is a heart attack".
- (August 2025). "Heart attack - Symptoms".
- (2022-01-07). "Relationship Between Body Posture and Lung Fluid Volume Assessed Using a Novel Noninvasive Remote Dielectric Sensing System". Circulation Reports.
- [https://www.medlineplus.gov/ency/article/000063.htm Heart attack first aid]. [[MedlinePlus]]. Retrieved December 3, 2006.
- [https://web.archive.org/web/20010915230827/http://www.nhlbi.nih.gov/actintime/index.htm Act In Time to Heart Attack Signs] - [[NHLBI]]. Retrieved December 13, 2006.
- Gheeraert, Peter. "Ventricular fibrillation during acute myocardial infarction".
- [http://www.ehac.org/st-agnes/EHAC_LifeandDeath/TimeisMuscle.htm TIME IS MUSCLE TIME WASTED IS MUSCLE LOST] {{webarchive. link. (December 17, 2000 . Early Heart Attack Care, St. Agnes Healthcare. Retrieved November 29, 2006.)
- (August 2004). "ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction--executive summary. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to revise the 1999 guidelines for the management of patients with acute myocardial infarction)". J. Am. Coll. Cardiol..
- [http://www.collegeofparamedics.org/Content_Files/Files/aocp_emtP.pdf Alberta Occupational Competency Profile EMT Paramedic] {{webarchive. link. (2011-10-05. [[Alberta College Of Paramedics]]. Updated January 2007, Retrieved June 29, 2011.)
- (July 2002). "Evaluation of the time saved by prehospital initiation of reteplase for ST-elevation myocardial infarction: results of The Early Retavase-Thrombolysis in Myocardial Infarction (ER-TIMI) 19 trial". J. Am. Coll. Cardiol..
- (2000). "Mortality and prehospital thrombolysis for acute myocardial infarction: A meta-analysis". JAMA.
- (2006). "Rationale for establishing regional ST-elevation myocardial infarction receiving center (SRC) networks". Am. Heart J..
- (June 2004). "Implications of the Mechanical (PCI) vs Thrombolytic Controversy for ST Segment Elevation Myocardial Infarction on the Organization of Emergency Medical Services: The Boston EMS Experience". Crit Pathw Cardiol.
- (April 2005). "Reduction of treatment delay in patients with ST-elevation myocardial infarction: impact of pre-hospital diagnosis and direct referral to primary percutanous coronary intervention". Eur. Heart J..
- (April 2006). "ST-segment elevation myocardial infarction: recommendations on triage of patients to heart attack centers: is it time for a national policy for the treatment of ST-segment elevation myocardial infarction?". J. Am. Coll. Cardiol..
- Rokos I. and Bouthillet T., {{usurped
- Cannon, Christopher. (1999). "Management of acute coronary syndromes". Humana Press.
- (2012). "Third universal definition of myocardial infarction". European Heart Journal.
- (1999). "Use of Sildenafil (Viagra) in Patients With Cardiovascular Disease". Circulation.
- (2016). "Oxygen therapy for acute myocardial infarction". The Cochrane Database of Systematic Reviews.
- (2013). "Goodman and Gilman Manual of Pharmacology and Therapeutics". McGraw-Hill Professional.
- (2013). "Drugs for the heart". Elsevier Saunders.
- (2014). "Reappraisal of thienopyridine pretreatment in patients with non-ST elevation acute coronary syndrome: a systematic review and meta-analysis". BMJ.
- [[ISIS-2]] Collaborative group. (1988). "Randomized trial of intravenous streptokinase, oral aspirin, both, or neither among 17,187 cases of suspected acute myocardial infarction: ISIS-2". Lancet.
- (2000). "Demographic, belief, and situational factors influencing the decision to utilize emergency medical services among chest pain patients. Rapid Early Action for Coronary Treatment (REACT) study". Circulation.
- (2004). "ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction)". J Am Coll Cardiol.
- Rossi S, editor. [[Australian Medicines Handbook]] 2006. Adelaide: Australian Medicines Handbook; 2006. {{ISBN. 0-9757919-2-3.
- (April 2009). "Management of patients with unstable angina / non-ST-elevation myocardial infarction: a critical review of the 2007 ACC /AHA guidelines". Int. J. Clin. Pract..
- (2012). "Relationship between treatment delay and final infarct size in STEMI patients treated with abciximab and primary PCI". BMC Cardiovasc Disord.
- (1995). "Predictors of 30-Day Mortality in the Era of Reperfusion for Acute Myocardial Infarction". Circulation.
- (1995). "Predictors of in-hospital and 6-month outcome after acute myocardial infarction in the reperfusion era: the Primary Angioplasty in Myocardial Infarction (PAMI) trail". J Am Coll Cardiol.
- (February 1994). "Indications for fibrinolytic therapy in suspected acute myocardial infarction: collaborative overview of early mortality and major morbidity results from all randomised trials of more than 1000 patients. Fibrinolytic Therapy Trialists' (FTT) Collaborative Group.". Lancet.
- (2006). "Aborted myocardial infarction: a new target for reperfusion therapy". Eur Heart J.
- (1991). "Mortality and morbidity in patients receiving encainide, flecainide, or placebo. The Cardiac Arrhythmia Suppression Trial". N Engl J Med.
- (1996). "Effect of d-sotalol on mortality in patients with left ventricular dysfunction after recent and remote myocardial infarction. The SWORD Investigators. Survival With Oral d-Sotalol". Lancet.
- (1997). "Randomised trial of effect of amiodarone on mortality in patients with left-ventricular dysfunction after recent myocardial infarction: EMIAT. European Myocardial Infarct Amiodarone Trial Investigators". Lancet.
- [https://www.nhlbi.nih.gov/health/heart-attack Life after a Heart Attack]. U.S. [[National Heart, Lung and Blood Institute]]. Retrieved December 2, 2006.
- Some patients become afraid of exercising because it might trigger another infarct.Trisha Macnair. [https://www.bbc.co.uk/health/conditions/heartattackrecovery1.shtml Recovering after a heart attack]. [[BBC]], December 2005. Retrieved December 2, 2006.
- (May 24, 2000). "Classification of Drivers' Licenses Regulations". Nova Scotia Registry of Regulations.
- link. (2010-07-22 Reviewed: 19 May 2010)
- "[http://familydoctor.org/002.xml Heart Attack: Getting Back Into Your Life After a Heart Attack] {{webarchive. link. (2008-07-24 ". [[American Academy of Family Physicians]], updated March 2005. Retrieved December 4, 2006.)
- (April 2008). "Management of cocaine-associated chest pain and myocardial infarction: a scientific statement from the American Heart Association Acute Cardiac Care Committee of the Council on Clinical Cardiology". Circulation.
- Faxon DP. (November 2005). "Coronary interventions and their impact on post myocardial infarction survival.". Clinical Cardiology.
- Youngwith, Janice. (2008-02-06). "Saving hearts in the air". Dailyherald.com.
- Dowdall N. (November 2000). ""Is there a doctor on the aircraft?" Top 10 in-flight medical emergencies.". BMJ (Clinical Research Ed.).
- (August 2007). "ACC/AHA 2007 guidelines for the management of patients with unstable angina/non ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non ST-Elevation Myocardial Infarction): developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons: endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation and the [[Society for Academic Emergency Medicine]]". Circulation.
- Cheitlin, Melvin. "Use of Sildenafil (Viagra) in Patients With Cardiovascular Disease".
- Cheitlin, Melvin. "Use of Sildenafil (Viagra) in Patients With Cardiovascular Disease". AHA.
- Bates ER. (2007). "Role of intravenous beta-blockers in the treatment of ST-elevation myocardial infarction: Of mice and men". Circulation.
- (1999). "Beta blockade after myocardial infarction: Systematic review and meta regression analysis". BMJ.
- Braunwald, E. (2012). ST-Segment Elevation Myocardial Infarction: Management. Braunwald's Heart disease: a textbook of cardiovascular medicine (9th ed., ). Philadelphia: Saunders.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Management of acute coronary syndrome — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report