From Surf Wiki (app.surf) — the open knowledge base
Dracunculus medinensis
Species of parasitic worm

Species of parasitic worm
the human parasite D. medinensis
Dracunculus medinensis (Guinea worm, dragon worm, fiery serpent) is a nematode that causes dracunculiasis, also known as Guinea worm disease. The disease is caused by the female which, at around 80 cm in length, is among the longest nematodes infecting humans. The length of specimens exhibits extreme sexual dimorphism, as the longest recorded male Guinea worm is only 4 cm.
Guinea worm disease is on target to be the second infectious disease of humans to be eradicated, after smallpox, and the D. medinensis species would be made extinct to accomplish it. It was formerly endemic to a wide swath of Africa and Eurasia; as of 2023, it remains endemic in five countries: Chad, Mali, South Sudan, Angola and Ethiopia, with most cases in Chad. Guinea worm spread to Angola , and it is considered endemic there. Infection of domestic dogs is a serious complication in Chad.
The common name "Guinea worm" is derived from the Guinea region of Western Africa.
History
Dracunculus medinensis ("little dragon from Medina") was described in Egypt as early as the and possibly was the "fiery serpent" afflicting the Israelites described in the Bible.
In the mid-19th century, the nematode Camallanus lacustris, which infects freshwater fish, was discovered to develop in copepods. This led Russian naturalist Alexei Pavlovich Fedchenko to discover in 1870 that D. medinensis is similarly transmitted via copepod intermediate hosts.
Life cycle

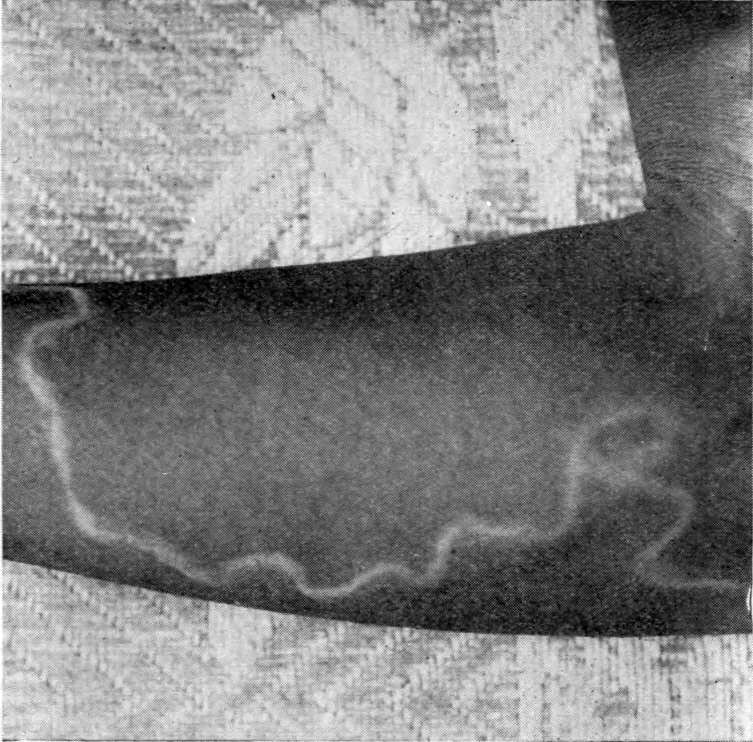
D. medinensis L1 larvae are found in fresh water, where they are ingested by copepods (small crustaceans) of the genus Cyclops. Within the copepod, the D. medinensis larvae develop to an infective L3 stage within 14 days. When the infected copepod is ingested by a mammalian host drinking unfiltered water, the copepod is then dissolved by stomach acid and dies and the D. medinensis larvae are released and migrate through the wall of the mammalian intestine, and enter the abdominal cavity and retro-peritoneal space, where they mature into adults. After maturing and mating within the host, the males die and females (length 60-100 cm or longer) | access-date = 2025-08-17 | url-status = live | archive-url = https://web.archive.org/web/20250721001335/https://www.who.int/news-room/fact-sheets/detail/dracunculiasis-(guinea-worm-disease) | archive-date = 2025-07-21 migrate in subcutaneous tissue towards the skin's surface. Around a year after the infection, the female causes the formation of a blister on the skin's surface, generally on the lower extremities, though occasionally on the hand or scrotum. When the blister ruptures, the female slowly emerges over the course of several days or weeks.
Animal reservoirs
In 2020, Guinea worm was found in 1,507 domestic dogs in Chad, 15 in Ethiopia, and eight in Mali, as well as in 61 domestic cats in Chad and three in Ethiopia. Small numbers have also been found in wildcats and baboons. These findings are a potential problem for the eradication program.
Epidemiology
D. medinensis is most commonly found in the subtropic to tropical regions, especially in India, south-west Asia (Iraq, Iran, Pakistan, etc.), and rural areas of Africa, where temperatures of 25-30 C are best for larval development. The parasite relies on people accidentally consuming microcrustaceans of the genus Cyclops (copepods), that dwell in stationary bodies of water such as ponds, large, open wells (with stairs), or rain-filled cisterns. The infection occurs most during times of drought or the "dry-season" in humid climates, or during or just after the rain season in the "semiarid, wet-and-dry-climates". This is due to the lower surface water of the stationary bodies of water, which are prime for the growth of the infected copepods, and main source of water for many.
Pathology
D. medinensis causes dracunculiasis as a result of the emergence of the female worm, non-emergence of adult worms (usually the male), and secondary bacterial infections. As it emerges to the subcutaneous tissue, the female releases a toxic chemical that may result in nausea, rash at site, diarrhea, dizziness, localized edema, reddish papule, blister, and itching. Arthritis or paraplegia can result from a worm that fails to reach the skin and gets calcified in or along the joint or finds its way into the central nervous tissue. Aseptic abscesses and cystic swelling can also occur when worms rupture before emerging, causing an acute inflammatory response from the host's immune system.
Treatment

The female Guinea worm slowly starts to emerge from the host's skin after the blister ruptures. The most common method for removing the worm involves submerging the affected body part in water to help coax the worm out. The site is then cleaned thoroughly. Then, slight pressure is applied to the worm as it is slowly pulled out of the wound. To avoid breaking the worm, pulling should stop when resistance is met. Full extraction of the female Guinea worm usually takes several days. After each day's worth of extraction, the exposed portion of the worm is wrapped around a piece of rolled-up gauze or small stick to maintain tension. This method of wrapping the worm around a stick or gauze is speculated to be the source for the Rod of Asclepius, the symbol of medicine. Once secure, topical antibiotics are applied to the affected region to help prevent secondary infections due to bacteria. The area is then wrapped in gauze to protect the wound. The same steps are repeated each day until the whole worm has been removed from the lesion.
Control & Prevention of the Parasite
| Year | Reported cases | Countries | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1986 | estimated | 21 | ||||||||
| 1989 | 892,055 | title=Dracunculiasis Epidemiological Data (1989-2008) | website=who.int | publisher=World Health Organization | url=https://www.who.int/dracunculiasis/epidemiology/Epidemiological_data.pdf | access-date=2009-09-14}} | ||||
| 1992 | 374,202 | 15 | ||||||||
| 1995 | 129,852 | 19 | ||||||||
| 2000 | 75,223 | 16 | ||||||||
| 2001 | 63,717 | 16 | ||||||||
| 2002 | 54,638 | 14 | ||||||||
| 2003 | 32,193 | 13 | ||||||||
| 2004 | 16,026 | 13 | ||||||||
| 2005 | 10,674 | 12 | ||||||||
| 2006 | 25,217 | 10 | ||||||||
| 2007 | 9,585 | 9 | ||||||||
| 2008 | 4,619 | 7 | ||||||||
| 2009 | 3,190 | 5 | ||||||||
| 2010 | 1,797 | title=Guinea worm countdown: The road to eradication | website=cartercenter.org | publisher=The Carter Center | url=http://www.cartercenter.org/health/guinea_worm/mini_site/current.html | access-date=2018-07-22 | archive-url=https://web.archive.org/web/20110906091154/http://www.cartercenter.org/health/guinea_worm/mini_site/current.html | archive-date=2011-09-06}} (6) | ||
| 2011 | 1,060 | title=Wrap-up #209 | date=9 January 2012 | periodical=Guinea Worm Wrap-up | issue=209 | series=WHO Collaborating Center for Research, Training and Eradication of Dracunculiasis | publisher=World Health Organization (WHO) | via=The Carter Center (cartercenter.org) | url=http://www.cartercenter.org/resources/pdfs/news/health_publications/guinea_worm/wrap-up/209.pdf }} | |
| 2012 | 542 | title=Wrap-up #218 | date=2013-04-22 | periodical=Guinea Worm Wrap-up | issue=218 | series=WHO Collaborating Center for Research, Training and Eradication of Dracunculiasis | publisher=World Health Organization (WHO) | via=The Carter Center (cartercenter.org) | url=https://www.cartercenter.org/resources/pdfs/news/health_publications/guinea_worm/wrap-up/218.pdf | access-date=2022-11-04}} |
| 2013 | 148 | title=Wrap-up #226 | date=2014-05-09 | periodical=Guinea Worm Wrap-up | issue=226 | series=WHO Collaborating Center for Research, Training and Eradication of Dracunculiasis | publisher=World Health Organization (WHO) | via=The Carter Center (cartercenter.org) | url=https://www.cartercenter.org/resources/pdfs/news/health_publications/guinea_worm/wrap-up/226.pdf | access-date=2022-11-04}} |
| 2014 | 126 | title=126 Cases of Guinea worm disease remain worldwide | date=11 January 2015 | website=cartercenter.org | publisher=The Carter Center | url=http://www.cartercenter.org/news/pr/gw-worldwide-cases-Jan2015.html | access-date=2015-05-09}} | |||
| 2015 | 22 | title=Wrap-up #240 | date=2016-05-13 | periodical=Guinea Worm Wrap-up | issue=240 | series=WHO Collaborating Center for Research, Training and Eradication of Dracunculiasis | publisher=World Health Organization (WHO) | via=The Carter Center (cartercenter.org) | url=https://www.cartercenter.org/resources/pdfs/news/health_publications/guinea_worm/wrap-up/240.pdf | access-date=2022-11-04}} |
| 2016 | 25 | author=Martin, Jeff | date=11 January 2017 | title=Carter: Guinea worm disease reported in 3 countries in 2016 | agency=Associated Press | url=http://bigstory.ap.org/article/13da4bec739e4886b06e63175b6a6ebf/carter-guinea-worm-disease-reported-3-countries-2016 | access-date=2017-01-11 | archive-date=12 January 2017 | archive-url=https://web.archive.org/web/20170112193945/http://www.bigstory.ap.org/article/13da4bec739e4886b06e63175b6a6ebf/carter-guinea-worm-disease-reported-3-countries-2016 | url-status=dead }} |
| 2017 | 30 | title=Announcement for 2017 Guinea worm disease case totals | date=19 January 2018 | website=cartercenter.org | publisher=The Carter Center | url=https://www.cartercenter.org/news/pr/guinea-worm-worldwide-cases-jan2018.html | access-date=2018-07-22 | url-status=live | archive-url=https://web.archive.org/web/20180120173342/https://www.cartercenter.org/news/pr/guinea-worm-worldwide-cases-jan2018.html | archive-date=2018-01-20}} |
| 2018 | 28 | 3 | ||||||||
| 2019 | 54 | title=54* cases of Guinea worm reported in 2019 | date=January 2020 | website=cartercenter.org | publisher=The Carter Center | url=https://www.cartercenter.org/news/pr/2020/guinea-worm-worldwide-cases-jan2020.html}} | ||||
| 2020 | 27 | 6 | ||||||||
| 2021 | 15 | 4 | ||||||||
| 2022 | 13 | 4 | ||||||||
| 2023 | 14 | 4 | ||||||||
| 2024 | 15 | 2 | ||||||||
| 2025 | 10 | 3 |
In the 1980s, the Carter Center initiated a program to eradicate the Guinea worm. The program included education of people in affected areas that the disease was caused by larvae in drinking water, isolation and support for affected people, and – crucially – widespread distribution of net filters and pipe filters for drinking water, and education about the importance of using them.
, the species has been reported to be near eradication. The International Commission for the Certification of Dracunculus Eradication has certified 198 countries, territories, and other WHO represented areas. As of January 2015, eight countries were yet to be certified as Guinea worm-free: Angola, the Democratic Republic of the Congo, Kenya, Sudan, Chad, Ethiopia, Mali, and South Sudan; of these, only in Chad, Ethiopia, Mali, and South Sudan does D. medinensis remain endemic.
, the disease has been reduced by more than 99.99% and more than 100 million cases have been prevented. | access-date = 2025-04-08 | url-status = live | archive-url = https://archive.wikiwix.com/cache/index2.php?url=https://www.cartercenter.org/news/pr/2025/2024-guinea-worm-worldwide-cases-announcement.html#federation=archive.wikiwix.com&tab=url | archive-date = 2025-04-08
Explanatory notes
References
References
- Chaudhury, Abhijit. (2022). "Textbook of Parasitic Zoonoses".
- (March 2008). "Antibody and cytokine responses in ''Dracunculus medinensis'' patients at distinct states of infection". [[Transactions of the Royal Society of Tropical Medicine and Hygiene]].
- Bimi, Langbong. (2007). "Potential vector species of Guinea worm (''Dracunculus medinensis'') in northern Ghana". Vector-Borne and Zoonotic Diseases.
- (2009). "Foundations of Parasitology". [[McGraw-Hill]].
- (2006). "'Serpent' in the breast". Journal of Ayub Medical College Abbottabad.
- Control of Neglected Tropical Diseases team. (2023). "Criteria for the certification of dracunculiasis eradication 2023 update". [[World Health Organization]].
- "Dracunculiasis: Historical background". [[World Health Organization]].
- Anderson, Roy C.. (8 February 2000). "Nematode Parasites of Vertebrates: Their development and transmission". CABI Publishing.
- "Dracunculiasis: About Guinea-Worm Disease". [[World Health Organization]].
- (2019). "Parasitic Diseases". Parasites Without Borders.
- (2020-09-17). "General information – frequently asked questions (FAQs)". U.S. [[Centers for Disease Control and Prevention]] (CDC).
- (26 January 2021). "Guinea worm cases fell 50% in 2020, Carter Center reports". [[The Carter Center]].
- Muller, R.. (1979). "Guinea worm disease: Epidemiology, control, and treatment". [[Bulletin of the World Health Organization]].
- (2012-11-27). "Gerald D. Schmidt & Larry S. Roberts' foundations of parasitology". [[McGraw Hill]].
- (2018-03-16). "Management of Guinea worm disease (GWD)". U.S. [[Centers for Disease Control]] (CDC).
- Satin, Morton. (2009). "Death in the Pot: The impact of food poisoning on history". Prometheus Books.
- "View Latest Worldwide Guinea Worm Case Totals". [[The Carter Center]].
- "Dracunculiasis Epidemiological Data (1989-2008)". [[World Health Organization]].
- (17 August 2007). "Progress toward global eradication of ''Dracunculiasis'', January 2005 – May 2007". U.S. [[Centers for Disease Control and Prevention]] (CDC).
- "Guinea worm countdown: The road to eradication". [[The Carter Center]].
- (4 March 2011). "Monthly report on dracunculiasis cases, January–December 2010". WHO.
- (9 January 2012). "Wrap-up #209". [[World Health Organization]] (WHO).
- (2013-04-22). "Wrap-up #218". [[World Health Organization]] (WHO).
- (2014-05-09). "Wrap-up #226". [[World Health Organization]] (WHO).
- (11 January 2015). "126 Cases of Guinea worm disease remain worldwide". [[The Carter Center]].
- (2016-05-13). "Wrap-up #240". [[World Health Organization]] (WHO).
- Martin, Jeff. (11 January 2017). "Carter: Guinea worm disease reported in 3 countries in 2016".
- (19 January 2018). "Announcement for 2017 Guinea worm disease case totals". [[The Carter Center]].
- (2019-05-06). "28 Guinea worm cases reported in 2018". [[The Carter Center]].
- (January 2020). "54* cases of Guinea worm reported in 2019". [[The Carter Center]].
- (2021). "Guinea worm cases fell 50% in 2020, Carter Center reports". [[The Carter Center]].
- (2022-03-31). "Wrap-up #286". [[World Health Organization]] (WHO).
- (2023-01-24). "Guinea worm disease reaches all-time low: Only 13* human cases reported in 2022".
- (2024-03-06). "Update: 14 Human Cases of Guinea Worm Reported in 2023".
- (2026-01-30). "Guinea Worm Disease Reaches All-Time Low: Only 10 Human Cases Reported in 2025".
- (2017-05-02). "Eradication program". U.S. [[Centers for Disease Control and Prevention]].
- (23 January 2015). "This species is close to extinction, and that's a good thing".
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about Dracunculus medinensis — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report