From Surf Wiki (app.surf) — the open knowledge base
ACTH stimulation test
Medical test to assess adrenal gland function
Medical test to assess adrenal gland function
| Field | Value | |
|---|---|---|
| Name | ACTH stimulation test | |
| Image | ||
| Caption | ||
| ICD10 | ||
| ICD9 | ||
| MeshID | ||
| MedlinePlus | 003696 | |
| OPS301 | ||
| LOINC | , | |
| synonyms | Synacthen test |
Name = ACTH stimulation test | Image = | Caption = | ICD10 = | ICD9 = | MeshID = | MedlinePlus = 003696 | OPS301 = | LOINC = , | synonyms = Synacthen test|
The ACTH test (also called the cosyntropin, tetracosactide, or Synacthen test) is a medical test usually requested and interpreted by endocrinologists to assess the functioning of the adrenal glands' stress response by measuring the adrenal response to adrenocorticotropic hormone (ACTH; corticotropin) or another corticotropic agent such as tetracosactide (cosyntropin, tetracosactrin; Synacthen) or alsactide (Synchrodyn). ACTH is a hormone produced in the anterior pituitary gland that stimulates the adrenal glands to release cortisol, dehydroepiandrosterone (DHEA), dehydroepiandrosterone sulfate (DHEA-S), and aldosterone.
During the test, a small amount of synthetic ACTH is injected, and the amount of cortisol (and sometimes aldosterone) that the adrenals produce in response is measured. This test may cause mild side effects in some individuals.
This test is used to diagnose or exclude primary and secondary adrenal insufficiency, Addison's disease, and related conditions. In addition to quantifying adrenal insufficiency, the test can distinguish whether the cause is adrenal (low cortisol and aldosterone production) or pituitary (low ACTH production). The insulin tolerance test is recognized as the gold standard assay of adrenal insufficiency, but due to the cumbersome requirement for a two-hour test and the risks of seizures or myocardial infarction, the ACTH stimulation test is commonly used as an easier, safer, though not as accurate, alternative. The test is extremely sensitive (97% at 95% specificity) to primary adrenal insufficiency, but less so to secondary adrenal insufficiency (57–61% at 95% specificity); while secondary adrenal insufficiency may thus be dismissed by some interpreters on the basis of the test, additional testing may be called for if the probability of secondary adrenal insufficiency is particularly high.
Adrenal insufficiency is a potentially life-threatening condition. Treatment should be initiated as soon as the diagnosis is confirmed, or sooner if the patient presents in apparent adrenal crisis.
Versions of the test
This test can be given as a low-dose short test, a conventional-dose short test, or as a prolonged-stimulation test.
In the low-dose short test, 1 μg of an ACTH drug is injected into the patient. In the conventional-dose short test, 250 μg of drug are injected. Both of these short tests last for about an hour and provide the same information. Studies have shown the cortisol response of the adrenals is the same for the low-dose and conventional-dose tests.
The prolonged-stimulation test, which is also called a long conventional-dose test, can last up to 48 hours. This form of the test can differentiate between primary, secondary, and tertiary adrenal insufficiency. This form of the test is rarely performed because earlier testing of cortisol and ACTH levels in association with the short test may provide all the necessary information.
Preparation
The test should not be given if on glucocorticoids or adrenal extract supplement, as these will affect test results. Stress and recently administered radioisotope scans can artificially increase levels and may invalidate test results. Spironolactone, contraceptives, licorice, estrogen, androgen (including DHEA) and progesterone therapy may also affect both aldosterone and cortisol stimulation test results. To stimulate aldosterone, consumption of salt should be reduced to a minimum, and foods high in sodium avoided for 24 hours prior to testing. Women should ideally undergo testing during the first week of their menstrual cycle as aldosterone (and occasionally cortisol) may be falsely elevated in the luteal cycle secondary to progesterone inhibition, leading to a compensatory rise in aldosterone levels.
Administration
Traditionally, cortisol and ACTH levels (separate lavender top tube) are drawn at baseline (time = 0). Next, synthetic ACTH or another corticotropic agent is injected IM or IV, depending on the agent. Approximately 20 mL of heparinized venous blood is collected at 30 and 60 minutes after the synthetic ACTH injection to measure cortisol levels.
ACTH samples are kept on ice and sent immediately to the laboratory, whereas cortisol does not need to be kept on ice.
Potential side effects
Commonly reported reactions are nausea, anxious sweating, dizziness, itchy skin, redness and or swelling of injection site, palpitations (a fast or fluttering heart beat), and facial flushing (may also include arms and torso), but should disappear within a few hours. Rarely seen, but serious side effects include rash, fainting, headache, blurred vision, severe swelling, severe dizziness, trouble breathing, irregular heartbeat.
Interpretation of results
Cosyntropin stimulation testing
In healthy individuals, the cortisol level should increase above 18–20 μg/dl within 60 minutes on a 250 mcg cosyntropin stimulation test.
For standardization across laboratories, the Short Synacthen Test is preferably performed in the morning (between 8:00 AM and 10:00 AM) to account for the diurnal peak of cortisol secretion. Baseline cortisol is drawn at time 0, with follow‑up samples at 30 minutes (and optionally 60 minutes) after administration of 250 μg synthetic ACTH. An adequate response is generally defined as a peak serum cortisol ≥ 500–550 nmol/L (approximately 18–20 μg/dL) or an increment ≥ 200 nmol/L, thresholds that improve diagnostic accuracy for adrenal insufficiency.
;Interpretation for primary adrenal insufficiency, Addison's disease In Addison's disease, both the cortisol and aldosterone levels are low, and the cortisol will not rise during the cosyntropin stimulation test.
;Interpretation for secondary adrenal insufficiency In secondary adrenal insufficiency, due to exogenous steroid administration suppressing pituitary production of ACTH or due to primary pituitary disorder causing insufficient ACTH production, the adrenal glands will atrophy over time and cortisol production will fall and patients will fail stimulation testing. Early in the development of secondary adrenal insufficiency, the adrenals may not have atrophied and can still stimulate, resulting in a normal cosyntropin stimulation test.
If secondary adrenal insufficiency is diagnosed, the insulin tolerance test (ITT) or the CRH (corticotropin-releasing hormone) stimulation test can be used to distinguish between a hypothalamic (tertiary) and pituitary (secondary) cause but is rarely used in clinical practice.
ACTH plasma test plus cortisol stimulation
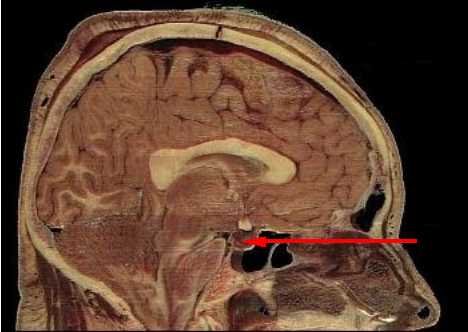
Measuring a morning, fasting ACTH level helps assess for the etiology of adrenal insufficiency.
;Interpretation for primary adrenal insufficiency and Addison's disease ACTH will be high – usually well above upper limits of reference range.
;Interpretation for secondary adrenal insufficiency ACTH will be low – usually below 35, but most people with secondary fall within the range limit. This is inappropriately normal for the low cortisol level.
In some cases, the actual cause of low ACTH is from low CRH in the hypothalamus. It is possible to have separate ACTH and CRH impairment such as can happen in a head injury.
Aldosterone stimulation
The ACTH stimulation test is occasionally used to test adrenal production of aldosterone at the same time as cortisol to also help in determining if primary (hyperreninemic) or secondary (hyporeninemic) hypoaldosteronism is present. Human ACTH has a slight stimulatory effect on aldosterone, but the amount of synthetic ACTH given in the stimulation is equivalent to more than a whole days production of natural ACTH, so the aldosterone response can be easily measured in blood serum. Same as cortisol, aldosterone should double from a respectable base value (around 20 ng/dl, must fast salt 24 hours and sit upright for blood draw) in a healthy individual.
;Interpretation for primary aldosterone deficiency The aldosterone response in the ACTH stimulation test is blunted or absent in patients with primary adrenal insufficiency including Addison's disease. The base value is usually in the mid-teens or less and rise to less than double the base value thus indicating primary hypoaldosteronism (sodium low, potassium and renin enzyme will be high) and is an indicator of primary adrenal insufficiency or Addison's disease.
;Interpretation for secondary aldosterone deficiency Aldosterone response of several factors from a low base value. This factoring indicates secondary hypoaldosteronism (sodium low, potassium and renin enzyme will be low). Usually doubling to quadrupling from a low base aldosterone value is what is seen in secondary adrenal insufficiency. Decoupling of aldosterone in the ACTH stimulation test is possible (i.e. 2 ng/dl stimming to 20). A result of doubling or more of aldosterone may help in tandem with a cortisol stimulation that doubled or more confirm a diagnosis of secondary adrenal insufficiency. In rare cases, an aldosterone stimulation which did not double, but with the presence of low potassium, low renin and low ACTH indicates atrophy of aldosterone production from the prolonged lack of renin.
Similar to the cortisol stimulation in ACTH deficiency, the test interpreter may lack knowledge of how to properly interpret for secondary hypoaldosteronism and think a result of aldosterone doubling or more from a low base value is good.
Future perspectives
Recent data showed that Synacthen test results can be used to predict future recovery of HPA axis function in patients with reversible causes of Adrenal Insufficiency.
Other hormones and chemicals that will rise in the ACTH stimulation test
- Progesterone – precursor to cortisol and aldosterone
- 17α-Hydroxyprogesterone – a progestogen steroid hormone related to progesterone
- Luteinizing hormone – a pituitary hormone that stimulates sex hormone production
- DHEA and DHEA-S – androgen hormones produced in the adrenal glands
Simple diagnostic chart
| **adrenal glands** | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| (primary)7 | high | high | high | high | low4 | low | high | low | high | tumor of the adrenal (adenoma), stress, antibodies, environment, Addison's, injury, surgical removal |
| ** 7** | Includes Addison's disease |
|---|
Veterinary medicine
The test is also used to diagnose hypoadrenocorticism in dogs and sometimes cats.
References
References
- (2003). "Diagnosis of adrenal insufficiency". [[Ann. Intern. Med.]].
- "ACTH stimulation test: MedlinePlus Medical Encyclopedia".
- (Nov 1995). "Selective increases in adrenal steroidogenic capacity during acute respiratory disease in infants.". Eur J Endocrinol.
- "ACTH Stimulation Test". Warde Medical Laboratory.
- "Synacthen Test". [[St George's Healthcare]].
- Ogbru, Omudhome. "Cosyntropin: Diagnositic Uses, Side Effects, Dosage".
- (2012-10-15). "Is the 250 μg ACTH test a useful tool for the diagnosis of central hypoadrenalism in adult patients with pituitary disorders?". Springer Science and Business Media LLC.
- "ADRENAL INSUFFICIENCY Chapter 13".
- (1999). "Comparison of the low dose short synacthen test (1 microg), the conventional dose short synacthen test (250 microg), and the insulin tolerance test for assessment of the hypothalamic-pituitary-adrenal axis in patients with pituitary disease". Journal of Clinical Endocrinology and Metabolism.
- (July 2010). "Comparison of low-dose and high-dose cosyntropin stimulation testing in children". [[Pediatrics International]].
- (2006). "Relationship between Aldosterone and Progesterone in the Human Menstrual Cycle". Journal of Clinical Endocrinology & Metabolism.
- "Cosyntropin (Professional Patient Advice)".
- "Rapid ACTH stimulation test diagnoses adrenal insufficiency".
- NIDDK's Office of Health Research Reports. "Addison's disease".
- (2016). "Diagnosis and Treatment of Primary Adrenal Insufficiency: An Endocrine Society Clinical Practice Guideline". The Journal of Clinical Endocrinology & Metabolism.
- Dg., Dayyal. (June 21, 2025). "Short Synacthen Test: Indication, Procedure, and Interpretation".
- Ashley B. Grossman. (2007). "Addison's Disease". Endocrine and Metabolic Disorders.
- Lynnette K Nieman. (2008). "Corticotropin-releasing hormone stimulation test".
- . ["Role of ACTH in Regulation and Action of Adrenocorticoids"](http://resources.med.fsu.edu/gsm/hp/program/section5/5ch7/s5ch7_7.htm).
- . ["Aldosterone and Renin"](http://www.labtestsonline.org/understanding/analytes/aldosterone/test.html).
- (1988). "Vasoactive intestinal peptide stimulates adrenal aldosterone and corticosterone secretion". [[Endocrinology (journal).
- link. (2018-06-15)
- (2000). "Stimulatory Effects of Stress on Gonadotropin Secretion in Estrogen-Treated Women*". The Journal of Clinical Endocrinology & Metabolism.
- (2017). "Congenital Adrenal Hyperplasia". Journal of Pediatric and Adolescent Gynecology.
- (2009). "Congenital adrenal hyperplasia". Dermato-Endocrinology.
- (2015). "Congenital adrenal hyperplasia due to 21-hydroxylase deficiency: A five-year retrospective study in the Children's Hospital of Damascus, Syria". Qatar Medical Journal.
- (2008). "Use of a low-dose ACTH stimulation test for diagnosis of hypoadrenocorticism in dogs.". Journal of Veterinary Internal Medicine.
- (November 1, 2008). "Consider ACTH stimulation test when you suspect canine hyperadrenocorticism". dvm360.com.
- "ACTH Stimulation Test". Idexx.
This article was imported from Wikipedia and is available under the Creative Commons Attribution-ShareAlike 4.0 License. Content has been adapted to SurfDoc format. Original contributors can be found on the article history page.
Ask Mako anything about ACTH stimulation test — get instant answers, deeper analysis, and related topics.
Research with MakoFree with your Surf account
Create a free account to save articles, ask Mako questions, and organize your research.
Sign up freeThis content may have been generated or modified by AI. CloudSurf Software LLC is not responsible for the accuracy, completeness, or reliability of AI-generated content. Always verify important information from primary sources.
Report